Let's talk about something that often gets whispered about but rarely discussed openly with enough detail: the signs of ovarian problems. It's a topic shrouded in worry, partly because the symptoms can be so vague. You feel a twinge in your side, some unusual bloating, or your periods just feel... off. Is it stress? Something you ate? Or could it be something more serious with your ovaries?
The truth is, ovarian issues span a wide spectrum, from harmless functional cysts that come and go, to endometriosis, polycystic ovary syndrome (PCOS), and the one that causes the most anxiety—ovarian cancer. The challenge, and the reason this guide exists, is that many of the warning signs overlap with common, everyday ailments. That persistent bloating you blame on lunch could be nothing. Or it could be a signal your body is sending that you shouldn't ignore. My aim here isn't to scare you, but to empower you with clear, actionable information. Think of this as your personal reference guide, written from the perspective of someone who's spent years sifting through the medical jargon to find the practical advice women actually need.
What's Inside This Guide
The Red Flag Symptoms You Can't Afford to Ignore
Some symptoms are like flashing neon signs. They demand immediate attention. If you experience any of the following, especially if they are new, persistent (lasting more than two weeks), and occur almost daily, consider it a non-negotiable cue to call your doctor.
Persistent Abdominal Bloating or Swelling
This isn't the "I had a big meal" bloat that comes and goes in a few hours. We're talking about a feeling of fullness, tightness, or visible swelling in your abdomen that doesn't really go away. It might even make your clothes feel tighter around the waist. In the context of ovarian problems, this can be caused by a large cyst, ascites (fluid buildup in the abdomen often linked to cancer), or simply the mass effect of a growth.
Pelvic or Abdominal Pain
This pain is a constant, dull ache or a feeling of pressure in your pelvis, lower back, or lower abdomen. It's different from sharp, intermittent menstrual cramps. A classic mistake is assuming all pelvic pain is gynecological. It can be, but it's also worth considering digestive or urinary causes. However, when combined with other symptoms on this list, the odds shift.
A sudden, severe, sharp pain in the pelvis is a medical emergency. It could indicate ovarian torsion (where the ovary twists on itself, cutting off blood supply) or a ruptured cyst. Don't wait this one out.
Feeling Full Quickly or Difficulty Eating
Medically termed 'early satiety,' this is when you feel unusually full after eating only a small amount of food. It's a sneaky symptom because you might just think your appetite has changed. This can happen if something in the pelvis is pressing on your stomach.
Urinary Symptoms: Urgency or Frequency
If you find yourself needing to urinate more often than usual or feeling a sudden, strong urge to go, pay attention. While a urinary tract infection (UTI) is the most common culprit, pressure from an ovarian mass on the bladder can produce identical sensations. If a course of antibiotics for a suspected UTI doesn't clear it up, it's time to look deeper.
The Subtle Signs: When "Normal" Isn't Normal Anymore
This is where it gets tricky. These signs are easy to dismiss because they mimic so many other conditions or are written off as just part of being a woman. The key is to look for a change from your personal baseline.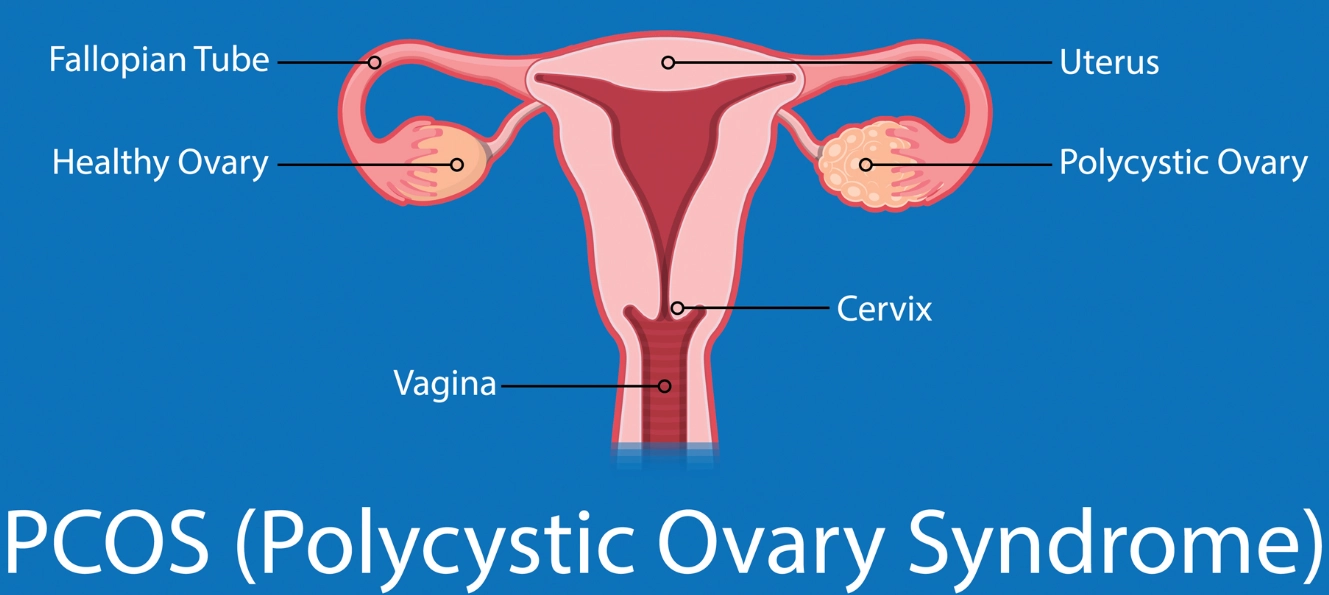
- Unexplained Fatigue: Not just "I didn't sleep well" tired, but a deep, unshakable exhaustion that rest doesn't fix.
- Changes in Bowel Habits: New constipation or diarrhea that isn't linked to diet changes. Pressure on the colon can alter its function.
- Unexplained Weight Loss or Gain: Losing weight without trying can be a sign of many illnesses. Gaining weight, especially around the abdomen, can be mistaken for simple weight fluctuation but may be related to fluid or a mass.
- Pain During Intercourse (Dyspareunia): Deep pain during or after sex can be a sign of ovarian cysts, endometriosis, or other pelvic issues.
- Menstrual Irregularities: Heavier, lighter, or more painful periods than usual, or bleeding between periods. While PCOS is a common cause, it's not the only one.
- Persistent Indigestion or Nausea: Another vague one that's often attributed to diet or stress.
I remember a friend who spent months treating what she thought was a stubborn case of IBS. The bloating and digestive issues were her only complaint. It was only when a sharp pain sent her to the ER that a large ovarian cyst was discovered. The lesson? Don't let a doctor (or yourself) settle for a superficial diagnosis if the treatment isn't working and your gut says something else is wrong.
What Could Be Causing This? Common Ovarian Conditions Explained
Not every sign points to cancer. Far from it. Most ovarian problems are benign. Understanding the landscape helps you have a more informed conversation with your doctor.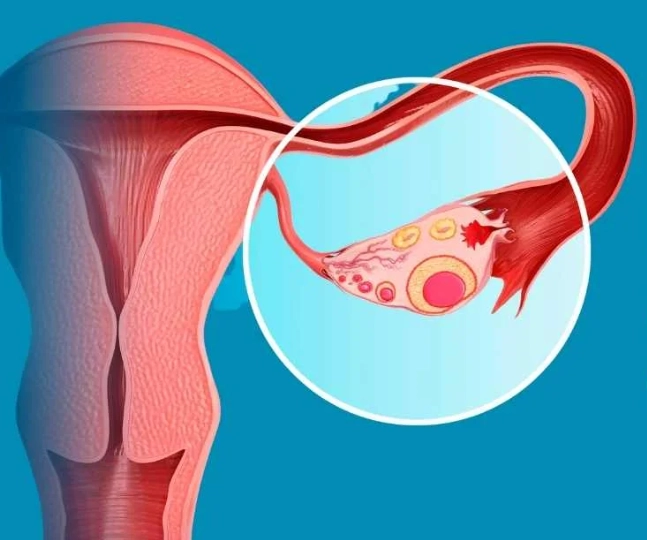
| Condition | Typical Signs & Symptoms | Key Notes |
|---|---|---|
| Ovarian Cysts (Functional, Dermoid, Cystadenomas) | Often none. If symptomatic: pelvic ache/bloating, pain during sex, frequent urination, menstrual irregularities. Sudden severe pain if ruptured or torsed. | Extremely common. Most are functional (related to the menstrual cycle) and resolve on their own in 1-3 months. Monitoring is the first step. |
| Polycystic Ovary Syndrome (PCOS) | Irregular/absent periods, excess hair growth, acne, weight gain, difficulty conceiving, pelvic pain (sometimes). | A hormonal disorder. Diagnosis requires specific criteria (Rotterdam criteria). Management focuses on symptoms and long-term metabolic health. |
| Endometriosis | Severe menstrual cramps, chronic pelvic pain, pain with sex, painful bowel movements/urination during periods, infertility, fatigue. | Endometrial-like tissue grows outside the uterus, often on ovaries. Pain level does NOT correlate with extent of disease. Laparoscopy is the gold standard for diagnosis. |
| Ovarian Cancer | The "red flag" cluster: persistent bloating, pelvic/abdominal pain, early satiety, urinary urgency/frequency. Also fatigue, back pain, changes in bowel habits. | Symptoms are often vague until later stages. There is no reliable screening test for average-risk women, making symptom awareness critical. |
How to Track Your Symptoms and When to See a Doctor
Walking into a doctor's office and saying "I have some pelvic pain" is less effective than providing a detailed log. Our memories are fuzzy, especially about discomfort. Here's a practical system:
Create a Symptom Log: Use a simple notes app or a small notebook. For two to four weeks, jot down:
- Symptom: (e.g., bloating, sharp left-side pain, urgency to urinate).
- Date & Time:
- Severity (1-10):
- What you were doing/eating:
- Relation to your menstrual cycle: Note the day of your cycle.
This log transforms vague complaints into concrete data. It can reveal patterns your doctor needs to see.
When to Make the Appointment
Don't use the "wait and see" approach for too long. Schedule an appointment with your gynecologist or primary care physician if:
- Any of the "red flag" symptoms are new and persist for more than two weeks.
- You experience sudden, severe pelvic pain.
- You notice a combination of subtle symptoms that represent a change for you and are affecting your quality of life.
- You have a family history of ovarian or breast cancer and are experiencing any persistent symptoms. Mention the family history upfront.
What to Expect at the Doctor
Be prepared. Bring your symptom log. The visit will likely include:
- A detailed conversation about your symptoms, health history, and family history.
- A pelvic exam to check for any masses or tenderness.
- Possible imaging: A transvaginal ultrasound is the primary tool to visualize the ovaries. It's non-invasive and can detect cysts, their characteristics, and other abnormalities.
- Blood tests: The CA-125 blood test is sometimes used. Crucially, CA-125 is NOT a screening test. It can be elevated in many non-cancerous conditions (endometriosis, fibroids, even menstruation). It's most useful as part of the diagnostic workup for a pelvic mass or for monitoring known ovarian cancer.
Your biggest job is to advocate for yourself. If you feel dismissed, ask specific questions: "What else could this be?" "Can we rule out an ovarian issue with an ultrasound?" "If this were your sister/daughter, what would you recommend?"





Leave a comment