Let's be real. If you're reading this, you're probably tired. Tired of the pelvic pain that feels like a constant, unwelcome guest. Tired of periods that knock you out for days. Tired of Googling "endometriosis medication" only to find the same vague lists that don't tell you what it's actually like to take these drugs. I get it. I've spent over a decade working with patients navigating this maze, and I've seen the same confusion and frustration repeat itself.
Endometriosis medication isn't about finding a magic pill. It's about building a strategic toolkit. The goal is control—over pain, over inflammation, over the growth of that misplaced tissue. And the landscape of options is more nuanced than just "take this for pain." The biggest mistake I see? People treating the symptom (pain) with over-the-counter meds while completely ignoring the underlying disease process. That's a fast track to more pain and progression.
Your Quick Navigation Guide
The Hormonal Arsenal: Slowing the Disease
Think of hormonal therapies as the foundation. They don't "cure" endometriosis, but they aim to slow or stop its growth by lowering estrogen levels or preventing ovulation. This is where long-term management happens.
Progestin-Based Therapies: Often the First Line
These are workhorses. Progestins counteract estrogen and can shrink lesions. Options range from daily pills (like norethindrone) to the Mirena IUD, which delivers hormone directly to the uterus. The IUD is a game-changer for many—it can drastically reduce period pain and bleeding for years. But here's the subtle error: starting with too low a dose. Many generic progestin pills start at a dose that's ineffective for endometriosis pain. You might need a higher dose, and it might take 3-6 months to see the full effect. Don't give up after six weeks.
Personal Observation: I've seen patients switch brands of the same progestin and have wildly different side effects. One might cause bloating, another might not. If the first one you try feels awful, it's worth discussing a different formulation with your doctor. It's not always the drug class, sometimes it's the specific compound or filler.
Combined Hormonal Contraceptives (The Pill, Patch, Ring)
The classic birth control pill, patch, or vaginal ring. By suppressing ovulation and creating a stable hormonal environment, they can prevent the monthly flare-ups. Taking them continuously (skipping the placebo week) is a common and effective strategy to stop periods altogether. But a major pitfall? Using a pill with a high-androgen progestin (like levonorgestrel) if you're already struggling with acne or mood swings. Opting for a pill with a low-androgen or anti-androgen progestin (like drospirenone) can make a world of difference in side effects.
GnRH Agonists and Antagonists: The Heavy Artillery
Drugs like Lupron (agonist) or Orilissa/Myfembree (antagonists). They induce a temporary, reversible medical menopause by drastically lowering estrogen. The pain relief can be profound. The catch? Side effects like hot flashes and bone density loss are real. The non-consensus view? The fear of these drugs is often overblown when used correctly. The key is add-back therapy—taking a low dose of progestin (and sometimes estrogen) alongside them. This combo mitigates most menopausal side effects and protects bones while keeping the pain relief. Many doctors don't emphasize this enough upfront, causing unnecessary anxiety.
Beyond Ibuprofen: Targeted Pain Management
Hormonal therapy manages the disease, but you still need tools for breakthrough pain. This is a two-tier system.
| Medication Type | How It Works for Endo | Key Consideration & Common Mistake |
|---|---|---|
| NSAIDs (Ibuprofen, Naproxen) | Reduces inflammation and prostaglandins (pain chemicals) released by endometriosis lesions. | Mistake: Taking them after pain peaks. They work best as a pre-emptive strike. Start taking your dose 1-2 days before your expected period or pain flare. |
| Prescription NSAIDs (Meloxicam, Celecoxib) | Stronger, longer-lasting anti-inflammatory effect. Some are easier on the stomach. | Not all are equal. Celecoxib may have a lower risk of stomach issues. Don't assume your doctor will start with the strongest one; sometimes a longer-acting standard dose works better. |
| Neuropathic Pain Agents (Gabapentin, Pregabalin) | Calms overactive nerves that can become sensitized by chronic inflammation and pain. | These are for nerve-type pain (burning, shooting, electric). They are not first-line for cramping. A huge error is using them alone without addressing inflammation first. |
Let's talk about opioids. In acute, post-surgical pain, they have a role. For chronic endometriosis management? They are a dead-end street. They do nothing for the inflammation, cause tolerance, and can actually worsen pain sensitivity over time (hyperalgesia). Relying on them is a sign your current plan isn't working and needs a complete overhaul.
The Unspoken Realities of Medication
This is the stuff that rarely makes it to the pamphlet.
The Timeline is Everything. Hormonal medications are not fast-acting painkillers. You must judge their success over 3-6 months, not 3-6 weeks. Mark your calendar. Track symptoms. Give them a real chance.
Side Effects are Negotiable. Spotting on a new pill? That often settles in 3 months. Debilitating headaches? That might mean this specific formulation isn't for you. You have more room to negotiate with your doctor than you think. "This side effect is unacceptable, what's our Plan B?" is a perfectly valid question.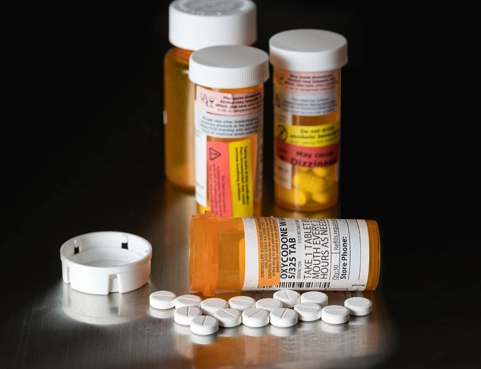
Red Flag: If a provider dismisses your reported side effects as "all in your head" or insists you stay on a medication that is severely impacting your quality of life without discussing alternatives, it's time to seek a second opinion. Patient advocacy groups like the Endometriosis Foundation of America stress the importance of a collaborative doctor-patient relationship.
Medication is Part of a Ecosystem. Pills alone often aren't enough. They work best paired with diet changes (reducing inflammatory foods), physical therapy for pelvic floor dysfunction (which almost always coexists), and stress management. Ignoring these is like trying to put out a fire with one hand while pouring gasoline with the other.
Finally, medication is a bridge, not always a forever solution. Its job is to control symptoms, improve your quality of life, and potentially slow progression so you can live well. For some, it's a long-term companion. For others, it's a tool used before or after surgery. The goal is to make the disease manageable, not let it manage you.




Leave a comment