If you think endometriosis is just about bad period cramps, you're missing the bigger, more complex picture. The reality is that endometriosis symptoms form a constellation of issues that can affect nearly every system in your body. I've spent years talking to patients and specialists, and the most common story I hear is one of dismissal—women being told their severe pain is "normal" or their fatigue is "just stress." Let's cut through that noise. This guide maps out the full terrain of endometriosis symptoms, from the classic signs to the ones that sneak up on you, so you can better understand what's happening in your body and advocate for yourself.
What's Inside This Guide?
The Biggest Myth About Endo Symptoms (And Why It's Dangerous)
Here's the non-consensus view that many mainstream resources gloss over: The severity of your pain does not correlate with the stage or extent of your endometriosis. You can have Stage IV, deep infiltrating endometriosis (DIE) and experience manageable discomfort. Conversely, you can have minimal, superficial lesions (Stage I) and be debilitated by excruciating pain. This disconnect is why so many people suffer for years without diagnosis—doctors often look for "severe disease" to explain severe symptoms, but that's not how this condition works.
The inflammation and nerve sensitization caused by endometriosis implants are the real drivers of pain, not necessarily the size or number of the implants themselves. This is a crucial piece of information to take into a doctor's appointment. If a physician suggests a laparoscopy isn't needed because your ultrasound was "clear," or downplays your pain because they assume mild disease, you now have the knowledge to push back. Your experience is valid, regardless of what imaging shows.
The Pain Spectrum: More Than Menstrual Cramps
Endometriosis pain is notorious for being dismissed as just a bad period. Let's break down the specific types, because precision matters when describing this to a healthcare provider.
1. Cyclical Pelvic Pain (Dysmenorrhea)
This isn't your average cramp. It often starts several days before your period and can last throughout. The pain is frequently described as deep, grinding, or throbbing, centered in the lower abdomen but often radiating to the lower back and thighs. Many women tell me it feels like their insides are being twisted or pulled apart. Over-the-counter ibuprofen often doesn't touch it.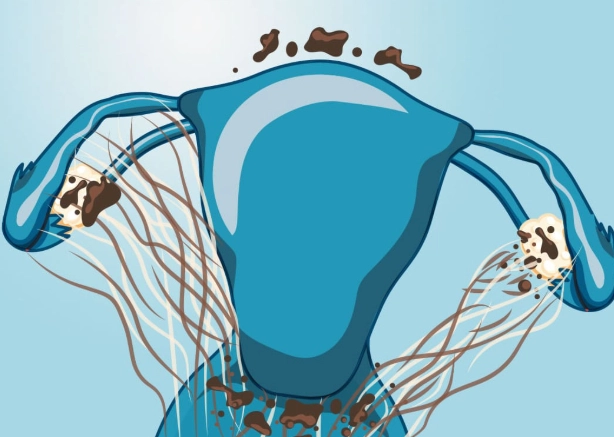
2. Pain During or After Sex (Dyspareunia)
This is a major red flag for deep infiltrating endometriosis, particularly if lesions are on the uterosacral ligaments or pouch of Douglas. The pain is typically deep and sharp, felt at the cervix or deep in the pelvis upon penetration. It's not a superficial friction issue. The aftermath can include cramping and spotting for hours or even days. This symptom alone destroys intimacy and relationships, and it's a huge, often silent, burden.
3. Painful Bowel Movements or Urination
When endometriosis affects the bowel (rectum, sigmoid colon) or bladder, it hijacks normal bodily functions. During your period, passing stool can feel like passing glass or cause severe, cramping rectal pain. Similarly, a full bladder can trigger sharp pain, and urination might sting. These symptoms are frequently misdiagnosed as irritable bowel syndrome (IBS) or recurrent UTIs.
Pro Tip for Tracking: Don't just note "pain." Describe it. Is it sharp, stabbing, burning, aching, cramping? Where exactly do you feel it? Does it radiate? What makes it better or worse? This level of detail is gold for a specialist.
Symptoms That Have Nothing to Do With Pain
This is where endometriosis shows its systemic nature. The inflammatory response it triggers doesn't stay localized to the pelvis.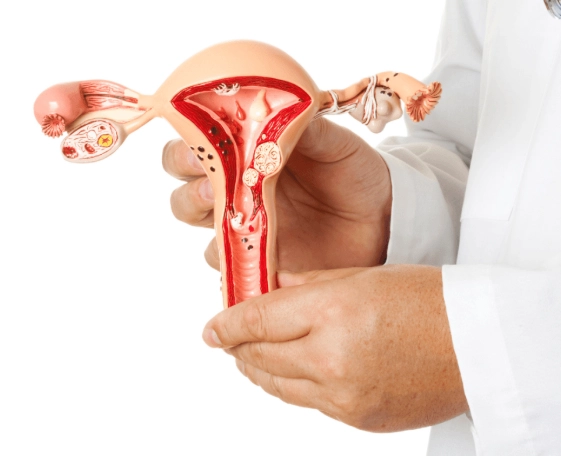
| Symptom Category | Specific Manifestations | Why It Happens |
|---|---|---|
| Fatigue | Overwhelming, unrelenting exhaustion that sleep doesn't fix. "Crashing" in the afternoon. | Chronic inflammation is an energy drain. The body is constantly trying to repair tissue. |
| Digestive Issues | Bloating ("endo belly"), nausea, diarrhea, constipation, alternating bowel habits. | Inflammation affecting the gut, hormonal influence on smooth muscle, or direct bowel involvement. |
| Heavy or Irregular Bleeding | Menorrhagia (soaking through products quickly), prolonged periods, spotting between cycles. | Inflammation and hormonal dysregulation affecting the uterine lining. |
| Mood & Cognitive Impact | Anxiety, depression, irritability, "brain fog," difficulty concentrating. | Inflammatory cytokines can cross the blood-brain barrier. Chronic pain is also mentally exhausting. |
"Endo belly" deserves its own mention. It's not just a little bloating. It's a distinct, often painful distention of the abdomen that can make you look several months pregnant within hours. It's caused by inflammation and fluid retention, and it's a hallmark sign that frustrates countless women when their clothes suddenly don't fit.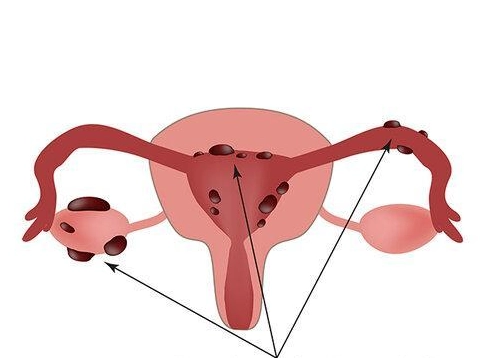
Lesser-Known and "Silent" Symptoms
Some symptoms are less common but equally telling. Others are "silent"—meaning you feel nothing, which is its own kind of problem.
Cyclical Shoulder or Chest Pain: This can indicate thoracic endometriosis, where tissue implants on the diaphragm or even in the lungs. The pain often coincides with your period.
Infertility: For many, infertility is the first and only symptom. Endometriosis can cause inflammation that's hostile to eggs and sperm, scar tissue (adhesions) that block tubes, and impair implantation. The Office on Women's Health notes that endometriosis is a leading cause of infertility.
Asymptomatic Endometriosis: Yes, it's possible. Some people only discover they have it during surgery for another issue, like a cyst or during a fertility work-up. This reinforces the point that symptom severity doesn't equal disease severity.
A Critical Note: If you experience sudden, severe abdominal pain, especially if accompanied by fever, vomiting, or fainting, seek emergency care immediately. This could indicate an ovarian cyst rupture (endometrioma) or another acute complication.
How Your Symptoms Behave: Patterns and Triggers
Symptoms aren't random. They follow patterns that, when recognized, become powerful diagnostic clues.
The Hormonal Link: Most symptoms are cyclical, worsening in the days leading up to and during menstruation when estrogen levels drop and inflammatory prostaglandins spike. However, with deep infiltrating or adhesive disease, pain can become chronic and constant, losing its clear cyclical pattern.
Common Triggers:
- Diet: For many, inflammatory foods like gluten, dairy, red meat, and processed sugars can flare symptoms within 24-48 hours.

- Stress: It's not "all in your head," but stress heightens systemic inflammation, which can turn up the volume on all your symptoms.
- Physical Activity: High-impact exercise or certain movements (like deep squats) can aggravate pelvic pain, while gentle movement like yoga or walking often helps.
- Full Bladder or Bowel: As mentioned, the pressure can be intensely painful if those organs are involved.
I recall one patient, Sarah, who for years thought her debilitating back pain was from a old sports injury. It was only when she connected the dots—that it reliably flared the week before her period and was accompanied by bloating and fatigue—that she sought a specialist and was diagnosed with endometriosis on her uterosacral ligaments.
From Symptoms to Action: Your Next Steps
Recognizing symptoms is step one. Acting on them is step two. Here’s a practical plan.
1. Start a Symptom Diary
Use an app or a notebook. Track for 2-3 cycles. Log: pain (type, location, intensity 1-10), bowel and bladder habits, energy levels, mood, bleeding, and any potential triggers (food, stress, activity). This creates objective data you can bring to a doctor.
2. Prepare for Your Doctor's Appointment
Don't go in saying "I have bad periods." Go in with your diary and a list. Say: "I experience deep pelvic pain that starts 5 days before my period and is an 8/10. I also have painful bowel movements during my cycle and debilitating fatigue. I've tracked this for three months." This changes the conversation.
3. Seek the Right Specialist
A general OB/GYN may not have the expertise. Look for a gynecologist who specializes in endometriosis or pelvic pain. Resources from organizations like the World Endometriosis Society can help you find specialists. Be prepared for a long wait—book the appointment now.
4. Understand the Diagnostic Challenge
Transvaginal ultrasound and MRI can detect cysts (endometriomas) and deep disease, but they often miss superficial implants. A "normal" scan does not rule out endometriosis. The gold standard for diagnosis is still a laparoscopy with biopsy. It's an imperfect system, but knowing this helps you navigate it.
Your Burning Questions, Answered
Can my endometriosis symptoms change or get worse as I get older?
They can, but not always in a linear way. Perimenopause is a wild card. While declining estrogen might ease symptoms for some, the hormonal fluctuations during this time can actually cause severe flares for others. Symptoms don't magically vanish at menopause if you have estrogen-producing implants or are on hormone therapy. The goal of treatment shifts to managing symptoms through this transition.
I was told I have IBS. Could it actually be endometriosis symptoms?
It's incredibly common. Studies suggest a significant overlap. The key differentiator is timing. If your bloating, diarrhea, and pain are consistently worse around your period, endometriosis involvement is highly suspect. Pure IBS is less tied to the menstrual cycle. It's also possible to have both conditions simultaneously. A specialist can help untangle this.
Is there a specific diet that helps manage endometriosis symptoms?
There's no one-size-fits-all diet, but an anti-inflammatory approach is the consensus starting point. Based on patient reports and some research, reducing or eliminating gluten, dairy, and processed foods helps many. Increasing omega-3s (fatty fish, flaxseed) and antioxidants (colorful fruits and vegetables) can combat inflammation. The trick is to do a strict elimination diet for 4-6 weeks, then reintroduce foods one by one to identify your personal triggers. It's work, but it's one of the few things within your direct control.
Can exercise make my endometriosis pain worse?
It depends entirely on the exercise and your body. High-intensity interval training (HIIT) or heavy lifting can increase intra-abdominal pressure and trigger pain for many. However, gentle, consistent movement like walking, swimming, yoga, or Pilates (focusing on pelvic floor relaxation, not intense core engagement) is often therapeutic. It reduces inflammation and stress hormones. Listen to your body—if an activity causes a flare, modify it or stop. "No pain, no gain" is a dangerous mantra for endo.
Why did my symptoms get worse after my laparoscopy?
This is a heartbreaking reality for some. If surgery isn't performed by an expert in excision (cutting out the tissue root and all), but instead uses ablation (burning the surface), it can leave disease behind and create new scar tissue (adhesions). This scar tissue can be as painful as the original endometriosis. It underscores the critical importance of choosing a surgeon skilled in advanced laparoscopic excision, not just any surgeon who offers the procedure.






Leave a comment