Let's be honest. The word "infertility" hits hard. One month turns into six, then a year. The excitement fades, replaced by a quiet, monthly dread. I remember staring at yet another negative test, feeling completely lost in a sea of medical jargon—IUI, IVF, ICSI. What do they even mean? Which one is right? And, the big one, can we afford it?
This guide won't offer false hope or sugarcoat the process. Instead, it's the roadmap I wish I'd had. We'll walk through every infertility treatment option, not just the famous ones, laying out the real costs, the actual success rates (not the clinic's best-case scenario), and the emotional toll no one talks about enough. Think of this as a conversation with a friend who's been through it, helping you move from feeling overwhelmed to feeling informed and in control.
What's Inside This Guide
- Understanding Infertility: It's More Than Just "Trying"
- Step 1: The Evaluation & Pre-Treatment Phase
- A Detailed Breakdown of Infertility Treatment Options
- The Financial Reality: Costs, Insurance, and Affordability
- How to Choose the Right Infertility Treatment for You
- Beyond the Procedure: Success Stories and Mindset Management
- Your Burning Questions Answered (FAQ)
Understanding Infertility: It's More Than Just "Trying"
First, let's define it. Medically, infertility is the inability to conceive after 12 months of regular, unprotected intercourse if you're under 35, or after 6 months if you're 35 or older. It also includes the inability to carry a pregnancy to live birth. The key takeaway? It's a medical condition, not a personal failing.
The causes are split roughly equally: one-third are due to female factors, one-third to male factors, and one-third are a combination or unexplained. That last one—unexplained infertility—is incredibly frustrating. All tests come back normal, but pregnancy doesn't happen. It's more common than you think and a valid reason to pursue treatment.
A Critical Point Everyone Misses: Many couples rush into aggressive treatments like IVF without fully exploring or correcting lifestyle and "soft" factors. I've seen it countless times. Issues like untreated mild endometriosis, a borderline sperm analysis that could improve with supplements and lifestyle changes, or even unmanaged stress that disrupts ovulation are often overlooked in the race to the IVF lab. A good specialist will investigate these avenues first.
Step 1: The Evaluation & Pre-Treatment Phase
Before any talk of injections or procedures, you need a map. This phase is about diagnosis.
For Women:
The workup usually involves tracking ovulation (blood tests, ultrasound), checking the fallopian tubes are open (a test called an HSG), and looking at the uterine cavity. An often-underutilized test is an anti-Müllerian hormone (AMH) blood test, which gives a rough estimate of your ovarian reserve (egg count).
For Men:
A semen analysis is non-negotiable. It checks sperm count, movement (motility), and shape (morphology). Guys, please don't feel sidelined. This is a team effort, and this test is straightforward and critical.
This phase can take 1-2 menstrual cycles. Use this time. Start taking prenatal vitamins (with folic acid), cut back on alcohol and caffeine, and try to manage stress. These small steps genuinely matter.
A Detailed Breakdown of Infertility Treatment Options
Treatments are a ladder. You typically start on the lower rungs, which are less invasive and less expensive, and move up as needed. Here’s what each rung really entails.
Lifestyle & Medication (Ovulation Induction)
This is for women who aren't ovulating regularly (like those with PCOS). Medications like Clomid or Letrozole are taken orally for 5 days each cycle to stimulate the ovaries to release an egg. It's often combined with timed intercourse. Success rates per cycle are modest (about 10-15%), but it's a logical first step for many. The main risk is a multiple pregnancy (twins).
Intrauterine Insemination (IUI)
Often called "the turkey baster method" (a crude but memorable description). Around the time of ovulation, a washed and concentrated sample of sperm is placed directly into the uterus via a thin catheter. This bypasses the cervix and gets more sperm closer to the egg.
When it works best: For mild male factor infertility, cervical issues, or unexplained infertility. It's frequently paired with ovulation-inducing medications.
The reality check: IUI success rates are highly dependent on the woman's age. For a woman under 35, it might be 10-20% per cycle. After 40, it drops to around 5% or less. Most clinics recommend trying 3-6 cycles before moving on.
In Vitro Fertilization (IVF)
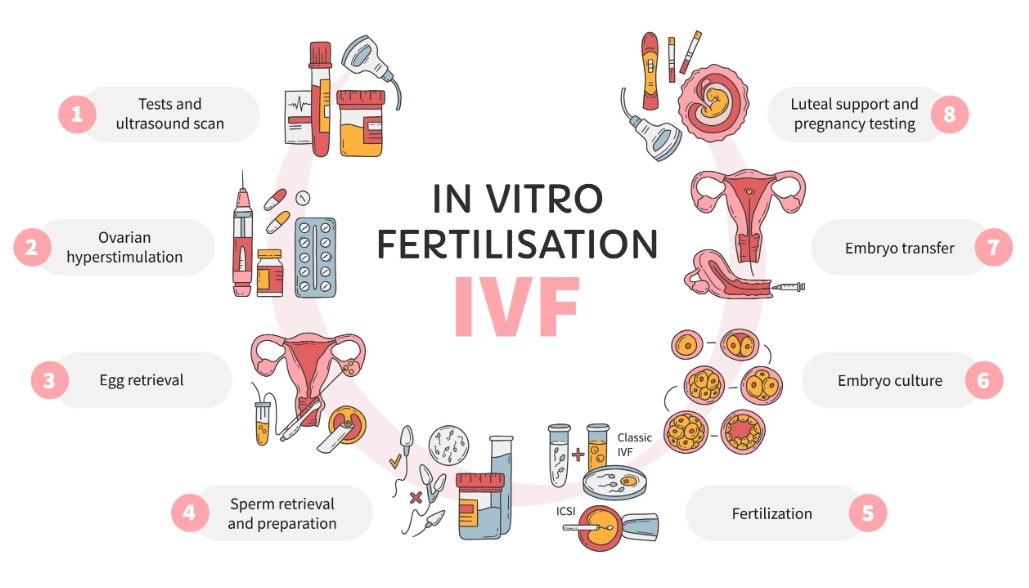
This is the big one. IVF involves stimulating the ovaries with daily injections to produce multiple eggs, retrieving those eggs in a minor surgical procedure, fertilizing them with sperm in a lab dish, and then transferring a resulting embryo (or embryos) back into the uterus.
It sounds intense because it is. The process takes about 2-3 weeks of active treatment per cycle. The physical side effects from the stimulation drugs (bloating, mood swings) are real. The emotional rollercoaster of waiting for fertilization reports and embryo updates is its own challenge.
Why it's so effective: It overcomes many barriers—blocked tubes, severe male factor (when paired with ICSI, where a single sperm is injected into an egg), endometriosis. It also allows for genetic testing of embryos (PGT-A).
Success rates are the highest of any treatment, but they are NOT 50/50 for most people. According to the latest CDC data, the percentage of IVF cycles resulting in a live birth for women using their own eggs is roughly:
- Under 35: 55%
- 35-37: 41%
- 38-40: 26%
- 41-42: 13%
- 43 and over: 4%
These are national averages. Clinic-specific rates can be found on the CDC's ART Success Rates website—a must-visit resource.
Surgical Options & Third-Party Reproduction
Sometimes the issue is structural. Surgery can remove fibroids, repair damaged tubes, or treat endometriosis. For some, using donor eggs, donor sperm, or a gestational surrogate is the path to parenthood. These are deeply personal decisions that come with their own emotional and ethical considerations.
| Treatment | Best For | Typical Process Duration | Average Cost Per Cycle (US) |
|---|---|---|---|
| Ovulation Induction + Timed Intercourse | Irregular/absent ovulation (e.g., PCOS) | 1 menstrual cycle | $500 - $2,500 (medications + monitoring) |
| Intrauterine Insemination (IUI) | Mild male factor, cervical issues, unexplained | 1 menstrual cycle | $1,000 - $4,000 |
| In Vitro Fertilization (IVF) | Tubal blockage, severe male factor, endometriosis, advanced maternal age, failed IUI | 2-3 weeks of active treatment | $12,000 - $25,000 (not including medications) |
The Financial Reality: Costs, Insurance, and Affordability
Let's talk money, because it's a massive barrier. The numbers in the table above are stark. IVF medications alone can cost $3,000 to $6,000 per cycle. Most people don't have $20,000 sitting in a savings account labeled "Baby Fund."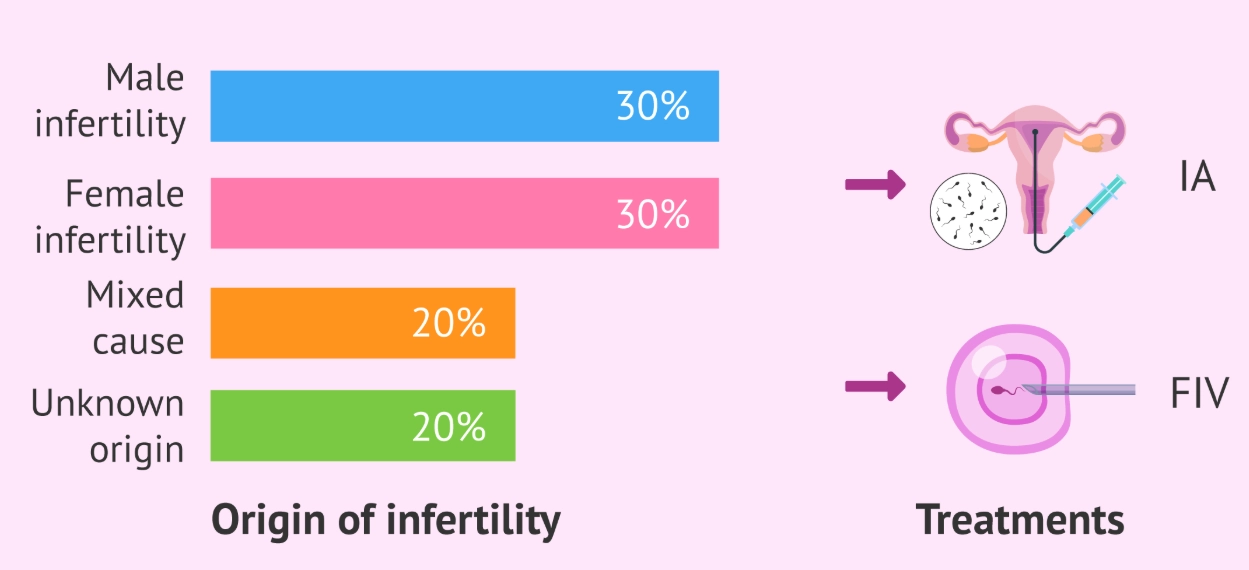
Insurance coverage is a patchwork. Some states have mandates requiring coverage for infertility diagnosis and treatment, but the specifics vary wildly. Other plans offer zero coverage. Your first call should be to your insurance company to ask for a summary of infertility benefits in simple language.
If you're paying out-of-pocket, explore all options:
- Clinic Shared-Risk or Refund Programs: You pay a larger lump sum (e.g., $30,000) for multiple IVF cycles. If you don't have a baby, you get a large portion refunded. High upfront cost, but can offer peace of mind.
- Medical Loans & Financing: Companies like Prosper Healthcare Lending specialize in this. Understand the interest rates.
- Grants & Scholarships: Organizations like Resolve: The National Infertility Association list financial resources. They are competitive but worth applying for.
Don't be shy about asking the clinic's financial counselor for a detailed, line-item cost estimate. A good clinic will be transparent.
How to Choose the Right Infertility Treatment for You
This isn't a one-size-fits-all decision. It's a Venn diagram of medical facts, emotional resilience, time, and finances.
Ask yourself and your partner these questions:
1. What is our specific diagnosis? The cause of infertility is the biggest driver. You can't fix blocked tubes with IUI.
2. How old are we (especially the female partner)? Age is the single greatest factor affecting egg quality and success rates. If you're 39, spending a year on low-probability IUIs might not be the best use of time.
3. What is our emotional and physical bandwidth? IVF is demanding. Are you prepared for daily injections, frequent clinic visits, and the potential for disappointment?
4. What is our financial ceiling? Be brutally honest. Going into severe debt can strain a relationship and add immense stress.
My personal, non-consensus advice? If you have unexplained infertility and are under 35, give 3-4 cycles of medicated IUI a real shot before leaping to IVF. The cost and burden are significantly lower. But if you're over 38, or have a clear diagnosis like severe male factor, going straight to IVF is often the most efficient (though costly) path. Discuss a clear "plan B" with your doctor. What will we do if 2 IUIs fail? Having a next step outlined reduces anxiety.
Beyond the Procedure: Success Stories and Mindset Management
Sarah, a friend I met in a support group, had three failed IUIs. She was drained. Her doctor suggested laparoscopic surgery on a hunch and found stage II endometriosis. After removal, she conceived naturally on her second cycle post-surgery. Her story isn't about a high-tech treatment; it's about a complete diagnosis.
Another couple, Mark and James, used IVF with donor eggs after years of trying with Mark's eggs and poor embryo quality. Their son is now two. Their success was about redefining their path to parenthood.
Protect your mental health. This journey can isolate you. Find your people—a therapist specializing in infertility, a support group (Resolve has great ones), or even a few trusted friends. Set boundaries with well-meaning but intrusive family. It's okay to skip the baby shower. Practice self-compassion. A failed cycle is not your fault.
Your Burning Questions Answered (FAQ)
 We can only afford one IVF cycle. How can we maximize our chances with that single shot?
We can only afford one IVF cycle. How can we maximize our chances with that single shot?



Leave a comment