Let's be direct. A diagnosis of infertility can feel like a wall. You've been trying, maybe for a year, maybe longer, and nothing. The internet is a maze of confusing terms—IVF, IUI, Clomid—and everyone seems to have an opinion. The good news? That wall has many doors. Modern infertility treatment is a spectrum, from simple lifestyle tweaks and targeted medications to sophisticated assisted reproductive technology (ART). The path isn't one-size-fits-all; it's built from a precise diagnosis of your specific situation. This guide cuts through the noise. We'll walk through the real steps, the actual costs (emotional and financial), the success rates you can realistically consider, and how to work with your doctor to map a plan that makes sense for you.
What's Inside This Guide
- How to Start: The Infertility Evaluation Process
- Navigating Female-Factor Infertility Treatments
- Addressing Male-Factor Infertility: It's Not Just About IVF
- Assisted Reproductive Technology (ART): IUI and IVF Explained
- How to Cope with the Emotional and Financial Cost of Infertility Treatment
- Your Fertility Treatment Questions, Answered
How to Start: The Infertility Evaluation Process
You don't start by picking a treatment. You start by getting answers. A formal evaluation, typically recommended after 12 months of unprotected sex (or 6 months if the female partner is over 35), is detective work. The goal is to identify any contributing factors. This isn't about blame; it's about creating a targeted strategy.
The process usually involves both partners from day one. A common and frustrating mistake I see is when the focus lands solely on the female partner for months before a basic semen analysis is done. Up to 30-40% of infertility cases involve male factors, either alone or combined with female factors, according to the American Urological Association. Skipping this step wastes time and emotional energy.
- For Her: A review of menstrual history, hormone blood tests (FSH, AMH, estradiol, thyroid), an ultrasound to check the uterus and ovaries, and an HSG (hysterosalpingogram) X-ray to see if the fallopian tubes are open.
- For Him: A semen analysis. This checks sperm count, motility (movement), and morphology (shape). It's non-invasive and provides crucial data.
- For Both: A detailed medical and lifestyle history. Things like thyroid disorders, past surgeries, medication use, smoking, alcohol, and weight can all play a role.
The results will point you toward a category: female-factor, male-factor, combined, or unexplained infertility (where all tests are normal). Unexplained doesn't mean untreatable; it means the treatment plan may be more empirical.
Navigating Female-Factor Infertility Treatments
Treatments here depend entirely on the diagnosed issue. Think of it as fixing specific parts of the conception assembly line.
Ovulation Disorders (The "When" Problem)
If you're not ovulating regularly, the first line is often oral medications like Clomiphene (Clomid) or Letrozole (Femara). These pills stimulate your ovaries. They're relatively low-cost and less invasive. But here's a subtle point many miss: monitoring is key. Taking the pills without follow-up ultrasounds to see how your follicles are developing is like driving blindfolded. You might over-respond (risk of multiples) or under-respond. Letrozole is often preferred for women with PCOS as some studies suggest better outcomes and lower twin rates.
Tubal or Uterine Factors (The "Where" Problem)
Blocked fallopian tubes or structural issues like fibroids or polyps? Surgery might be an option to repair tubes or remove growths. However, if tubes are severely damaged, success rates with surgery can be low. In many cases, this diagnosis leads directly to the recommendation for IVF, which bypasses the tubes entirely by fertilizing the egg in the lab.
Diminished Ovarian Reserve (The "Egg Supply" Problem)
This refers to a lower quantity or quality of eggs, often related to age. Treatments can't create more eggs, but they aim to make the best use of the existing reserve. This often involves more aggressive ovarian stimulation with injectable hormones (gonadotropins) followed by IVF to retrieve and fertilize as many eggs as possible. Time becomes a critical factor.
Addressing Male-Factor Infertility: It's Not Just About IVF
The old idea was that male infertility only led to donor sperm or IVF. Not anymore. A low sperm count or poor motility has its own treatment ladder.
First, lifestyle and medical fixes. A urologist specializing in male fertility can check for varicoceles (enlarged veins in the scrotum, which can be surgically repaired), hormone imbalances, or infections. Simple changes—avoiding hot tubs, reducing alcohol, quitting smoking, managing stress—can sometimes improve parameters in 3-6 months.
Then, procedural help. Even with suboptimal numbers, pregnancy might be possible by giving sperm a head start.
| Treatment | How It Works | Best For | Typical Cost Range (USD) |
|---|---|---|---|
| Intrauterine Insemination (IUI) | Sperm is washed and concentrated, then placed directly into the uterus around ovulation. | Mild male factor, cervical issues, unexplained infertility. | $500 - $1,500 per cycle |
| In Vitro Fertilization (IVF) with ICSI | A single sperm is injected directly into an egg in the lab. Bypasses most sperm quality issues. | Severe male factor, previous IVF fertilization failure. | $15,000 - $30,000+ per cycle |
ICSI (Intracytoplasmic Sperm Injection) revolutionized male infertility treatment. It requires just one viable sperm per egg. For men with extremely low counts, sperm can even be retrieved surgically from the testicle (TESE) for use with ICSI.
Assisted Reproductive Technology (ART): IUI and IVF Explained
When simpler interventions aren't enough or appropriate, ART steps in.
What is IUI (Intrauterine Insemination)?
Think of IUI as a targeted delivery service. It places washed, concentrated sperm directly into the uterus right when you ovulate, either naturally or with medication. It's less invasive and cheaper than IVF. Success rates per cycle are modest, often quoted between 10-20%, depending on age and diagnosis. It's frequently tried for 3-6 cycles before moving to IVF if unsuccessful.
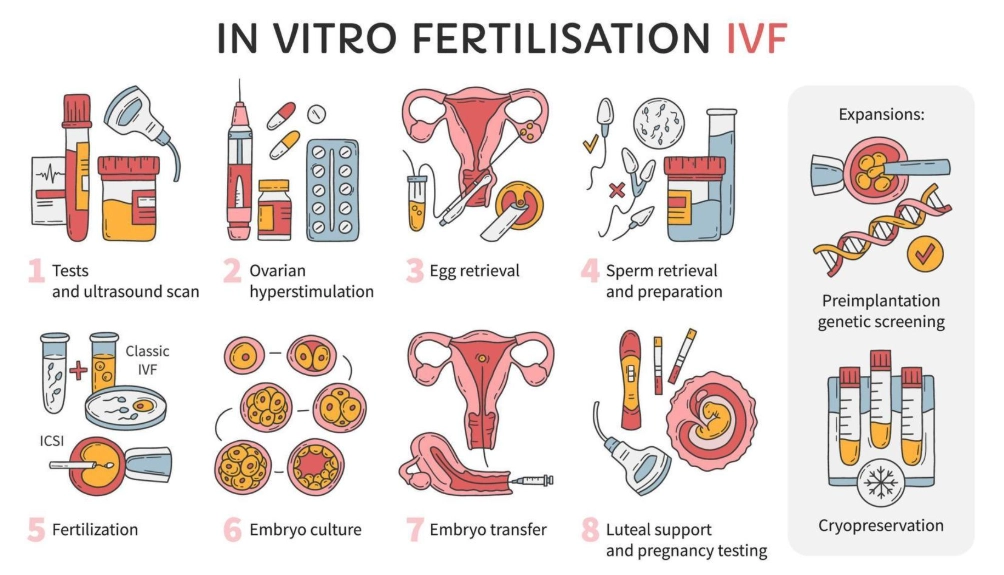
What Are the Steps of IVF (In Vitro Fertilization)?
IVF is a multi-step process over about 4-6 weeks. Understanding the phases demystifies it.
1. Ovarian Stimulation & Monitoring: You'll inject hormone medications for 8-12 days to stimulate multiple eggs to grow. You'll have frequent monitoring ultrasounds and blood tests. This is the most time-intensive phase.
2. Egg Retrieval: A minor surgical procedure under sedation. A doctor uses an ultrasound-guided needle to collect eggs from your ovaries. It takes about 20-30 minutes.
3. Fertilization & Embryo Development: In the lab, eggs are mixed with sperm (conventional IVF) or injected with a single sperm (ICSI). The fertilized eggs (now embryos) are cultured for 3-6 days.
4. Embryo Transfer: One (or sometimes two) healthy embryos are selected and placed into your uterus using a thin catheter. This is a quick, usually painless procedure.
5. The Two-Week Wait & Pregnancy Test: You'll take progesterone supplements to support the uterine lining and wait about 9-14 days for a blood pregnancy test.
Success rates for IVF vary dramatically by age. According to the CDC's ART Success Rates reports, for women under 35 using their own eggs, the live birth rate per egg retrieval is around 50-55%. This drops to about 40% for ages 35-37, 25% for ages 38-40, and under 10% for ages 42-44. These numbers are why age is the single biggest factor in treatment planning.
How to Cope with the Emotional and Financial Cost of Infertility Treatment
No one talks about this enough: infertility treatment is a marathon on a rollercoaster. The physical demands of injections and appointments are one thing. The emotional whiplash of hope, waiting, and potential disappointment each month is another. It can strain even the strongest relationships.
Financially, it's a burden. One IVF cycle can cost as much as a new car, and insurance coverage in the US is a patchwork. Many couples finance treatment through loans, grants (like from the RESOLVE organization), or shared-risk programs.
My advice? Build your support team early. This includes a therapist who specializes in infertility. Communicate openly with your partner—you may cope differently. Set emotional and financial boundaries before starting a cycle. Decide, for example, "We will try three IUIs before reassessing." Or "This is our budget; we will not go into debilitating debt." Having a plan B or C (like moving to donor eggs, adoption, or choosing a child-free life) can relieve the unbearable pressure of feeling like each cycle is your only chance.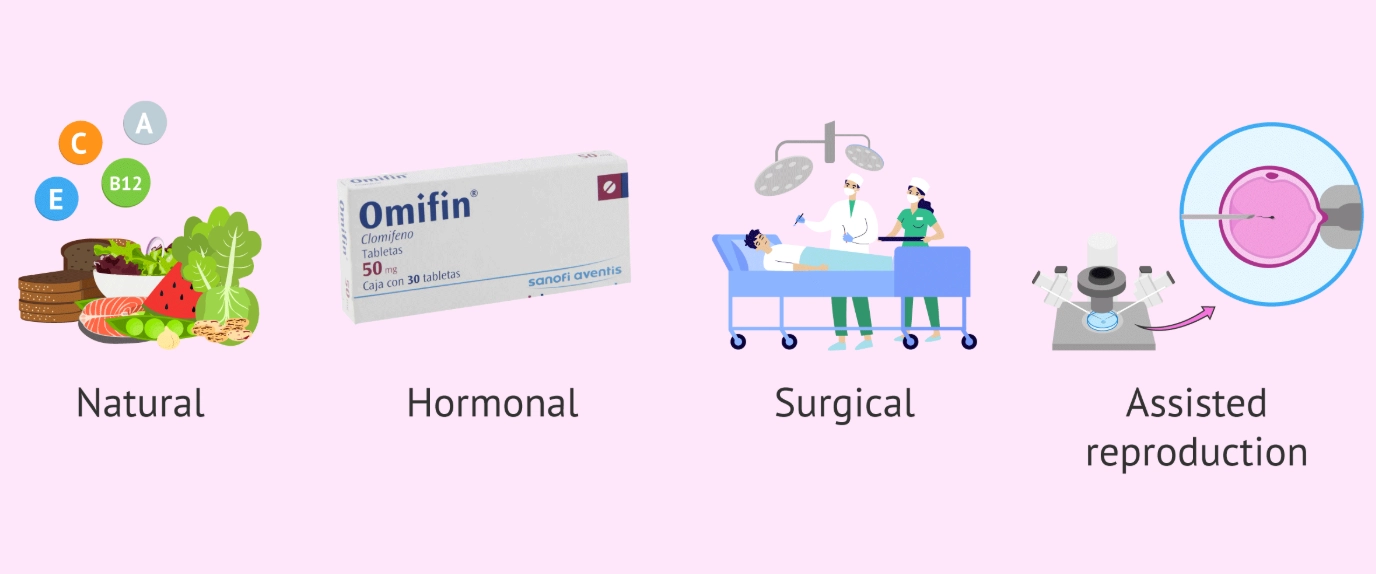
Your Fertility Treatment Questions, Answered
What is the most common mistake couples make when starting infertility treatment?
Failing to get a complete, simultaneous workup for both partners. Spending months treating the female partner for ovulation issues when the male partner has a severe sperm problem is a classic, time-wasting error. Insist on a semen analysis as part of the initial evaluation.
Is male infertility treatment just about getting to IVF with ICSI?
Absolutely not. While ICSI is a powerful tool, it's not step one. A consultation with a reproductive urologist can identify reversible issues like varicoceles or hormonal imbalances. Lifestyle changes and specific medications can sometimes improve sperm parameters enough to allow for less invasive treatments like IUI, or even natural conception, saving significant cost and physical burden.
 I'm 39 with a low AMH. Should I even bother with treatment, or go straight to donor eggs?
I'm 39 with a low AMH. Should I even bother with treatment, or go straight to donor eggs?
Are there any "natural" infertility treatments that actually work?
"Natural" is a loaded term. No supplement or diet will unblock a fallopian tube. However, lifestyle optimization is a valid and crucial part of any treatment plan. For both partners, achieving a healthy BMI, quitting smoking, reducing alcohol, managing stress, and taking a basic prenatal vitamin (with folic acid for her) can improve the body's environment for conception. Think of it as foundational work that supports medical treatment, not replaces it.
How do we handle the strain treatment puts on our relationship and intimacy?
Schedule sex that isn't just for procreation. Go on a date where talking about treatment is banned. See a counselor together, preferably one who understands infertility. Remember, you and your partner are on the same team against the problem, not against each other. The process can feel mechanical—injections, timed intercourse, procedures. Actively protecting moments of connection that have nothing to do with making a baby is essential for surviving the journey together.





Leave a comment