If you typed that question into Google, you’re probably hoping for a simple, one-word answer. Something like “IVF” or “IUI.” I get it. When you’re in the thick of fertility struggles, you want a clear winner, a champion treatment to pin your hopes on. But here’s the truth I’ve learned after years of working with patients and digging into the data: there is no single “most successful” treatment for everyone. The real answer is deeply personal and depends entirely on two things: how you define “success,” and the specific reasons behind your infertility.
Think of it this way. Asking for the most successful infertility treatment is like asking for the best car. For a family of five, it’s a minivan. For a solo commuter in a crowded city, it might be an electric scooter. Success is contextual.
So, let’s move beyond the oversimplified rankings and get into what actually matters. We’ll break down the real-world success rates of every major option, explain why your personal profile is the biggest factor, and give you a framework to find your most successful path forward.
Your Quick Guide to Navigating This Article
How Do You Define “Success” in Infertility Treatment?
This is the most critical, and most often overlooked, starting point. Clinics and studies throw around different metrics, and they’re not all created equal.
- Clinical Pregnancy Rate: This means a pregnancy confirmed by ultrasound (seeing a gestational sac). It’s a common benchmark, but it doesn’t account for miscarriages.
- Live Birth Rate: This is the gold standard. It tells you the percentage of treatment cycles that result in an actual baby being born. Always, always look for this number first.
- Cumulative Success Rate: This is a more helpful long-term view. It measures your chance of having a live birth after completing multiple treatment cycles (e.g., after 3 rounds of IVF). This number is almost always higher than the single-cycle success rate.
Here’s a mistake I see all the time. A couple gets excited by a clinic’s high “pregnancy rate,” only to be devastated by a later loss. The emotional and financial toll is immense. Focus on live birth rates. They tell the whole story.
A Realistic Breakdown of Major Infertility Treatments
Now, let’s look at the contenders. The table below uses generalized live birth rate data, primarily from the U.S. Centers for Disease Control and Prevention (CDC) National ART Surveillance System and clinical guidelines. Remember, these are averages and your mileage will vary dramatically.
| Treatment | Best For... | Typical Live Birth Rate (Per Cycle)* | Key Considerations |
|---|---|---|---|
| In Vitro Fertilization (IVF) | Blocked tubes, severe male factor, endometriosis, unexplained infertility, advanced maternal age, genetic screening. | ~20-40% (varies hugely with age) | Highest success per cycle for many causes; also the most invasive and expensive. Success heavily age-dependent. |
| Intrauterine Insemination (IUI) | Unexplained infertility, mild male factor, cervical issues, ovulatory disorders (when combined with medication). | ~10-20% (per cycle with meds) | Less invasive and cheaper than IVF. Success rates drop significantly after 3-4 cycles. Often a first-line treatment. |
| Fertility Medications (e.g., Clomid, Letrozole) | Ovulation disorders (like PCOS). | ~5-12% (live birth per cycle)** | Simple, low-cost oral pills. Only works if ovulation is the main issue. Requires monitoring. |
| Surgery (e.g., for fibroids, endometriosis) | Specific anatomical problems like large fibroids, scar tissue, or hydrosalpinx. | Varies widely | Can be curative for the specific issue, allowing for natural conception afterward. Not for all causes. |
* Rates are per initiated cycle for IVF/IUI, in women under 35. They fall sharply after age 37. ** Medication success is often measured in terms of ovulation or pregnancy; live birth data is less commonly isolated but is lower.
Looking at the table, IVF often has the highest per-cycle success rates for a broad range of issues. That’s why it frequently tops “most successful” lists. But that’s a massive oversimplification.
For a 29-year-old woman with polycystic ovary syndrome (PCOS) who isn’t ovulating, a few cycles of Letrozole might have a cumulative live birth chance of over 50%—at a fraction of the cost and stress of IVF. For her, medication is the most successful treatment. For a 42-year-old woman with diminished ovarian reserve, even IVF has sobering success rates (often under 10% per cycle), and IUI or medication alone would be statistically far less likely to work.
Beyond the Big Names: Other Paths to Success
Sometimes success isn’t about a medical procedure at all.
Lifestyle Modifications: For couples with obesity, smoking, or extreme stress, meaningful lifestyle changes can be the most successful intervention. One study in the journal Fertility and Sterility found that a structured lifestyle program could significantly improve natural conception rates in certain groups.
Donor Eggs or Sperm: When the issue is severe egg or sperm quality, using donor gametes can skyrocket the success rate of IVF, often to over 50% per transfer regardless of the recipient’s age. It’s a emotionally complex path, but from a pure statistical standpoint, it can be the most successful route to a live birth.
The #1 Thing That Determines Your Success: You
The treatment is just the tool. The raw material—your unique biology and circumstances—is what determines if that tool works. Here’s what really moves the needle:
- Female Age: This is the elephant in the room. Egg quantity and quality decline predictably. A woman’s age is the single strongest predictor of success with any treatment involving her own eggs. A clinic’s 40% IVF success rate is for women under 35. For women 41-42, that number might be 12%.
- The Root Cause of Infertility: Success rates for the same treatment differ wildly based on diagnosis. IVF success for tubal factor is generally higher than for severe male factor (though ICSI has largely closed that gap). Unexplained infertility can be frustrating because there’s no clear target.
- Lifestyle and Health: Smoking cuts IVF success rates nearly in half. A high BMI can affect ovulation, embryo quality, and medication response. Managing conditions like thyroid disease or diabetes is non-negotiable.
- Clinic and Lab Expertise: Not all clinics are equal. Embryologist skill, lab conditions, and protocol personalization matter. The CDC and the Society for Assisted Reproductive Technology (SART) publish clinic-specific success data—use it.
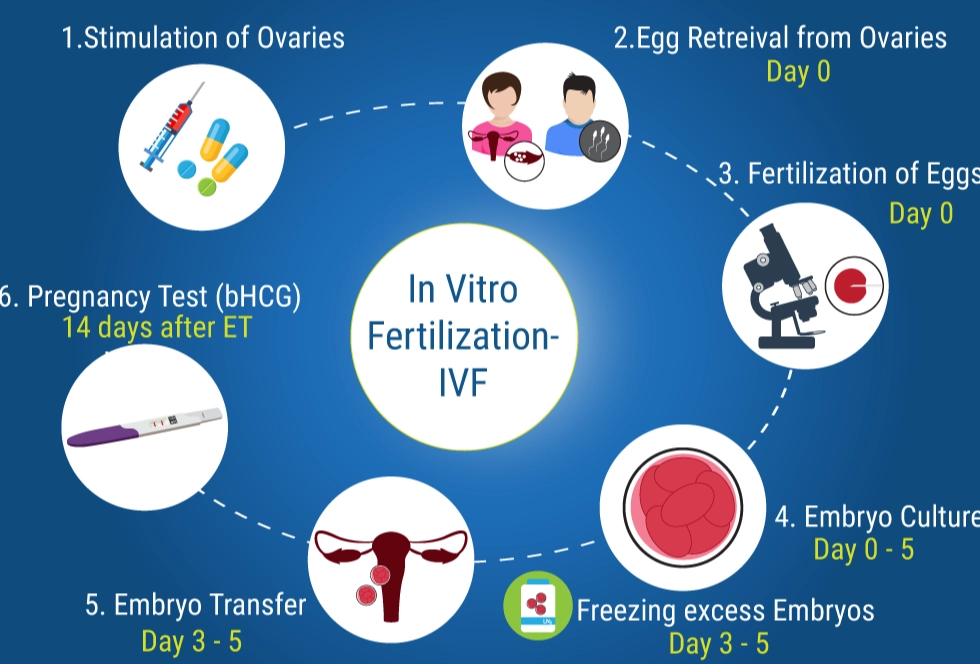
How to Choose the Right Infertility Treatment for You?
So how do you find your most successful treatment? Follow these steps. Don’t skip the first one.
1. Get a Clear Diagnosis. You can’t choose the right path if you don’t know where you’re starting from. This means a full workup: semen analysis, hormone testing, HSG or Sono to check tubes, ovarian reserve testing (AMH, AFC). “Unexplained” is a valid diagnosis, but only after everything else is ruled out.
2. Have a Blunt Conversation About “Success.” With your partner and your doctor, define what success means. Is it the highest chance per month? The least invasive option first? The most cost-effective path to a live birth? Getting on the same page is crucial.
3. Run the Numbers For YOUR Scenario. Don’t look at national averages. Ask your doctor: “Based on my age of 38, my AMH of 1.2, and my partner’s mild male factor, what is the estimated live birth rate per IVF cycle here? How does that compare to 3 cycles of IUI with injectable medications?” Get the data personalized.
4. Conduct a Cost-Benefit Analysis (The Real One). Factor in everything: financial cost, emotional toll, time off work, physical demands. A treatment with a slightly lower per-cycle success rate might be your “most successful” if you can afford to do it three times without bankrupting your family or your mental health.
5. Trust, But Verify, Your Clinic. Choose a clinic where you feel heard and that has expertise in your specific issue. Cross-reference their reported SART/CDC success rates with your personal estimates.
Your Top Fertility Treatment Questions, Answered
 We can only afford one treatment cycle. Should we go straight for the “most successful” one (IVF)?
We can only afford one treatment cycle. Should we go straight for the “most successful” one (IVF)?The journey to find the most successful infertility treatment is not about finding a magic bullet. It’s about matching the most effective tool to the unique blueprint of your life, your body, and your goals. Start with a precise diagnosis, insist on personalized live birth data, and weigh all the costs—not just the financial ones. Your most successful path is the one that leads you, sustainably and sanely, to your family.



Leave a comment