You feel it first in your temples – a tight, pounding headache. Maybe there's a wave of dizziness, or your vision seems a bit off. You check your blood pressure monitor, and the numbers stare back: 170/110, 180/115. Panic starts to creep in. What do you do right now? Before you reach for the phone or make a potentially dangerous move, take a deep breath. This guide is for that exact moment. Managing a sudden blood pressure spike at home is about calm, controlled actions, not magic cures. The immediate goal isn't to diagnose or replace a doctor, but to safely navigate the next 30-60 minutes while you assess whether you're facing a true hypertensive emergency. Let's walk through what actually works, what doesn't, and the critical signs that mean you need to stop reading and call 911.
What You'll Find in This Guide
Understanding the Goal: Calm, Not Cure
First, a reality check from someone who's counselled patients through this for years. Your body is in a stress response – “fight or flight.” Your blood vessels are constricted, your heart is working harder. The single most effective thing you can do at home is to break that stress cycle. You're not trying to drop your pressure from 180 to 120 in ten minutes. That kind of rapid drop can be dangerous in itself. You're aiming for a gradual reduction of 10-20 points over the next hour, and more importantly, you're preventing it from climbing higher while you figure out the next step.
Think of it like calming a startled animal. Sudden movements or loud noises (like panicking and taking extra medication) will make it worse. Quiet, predictable, soothing actions are key.
The Non-Consensus Truth: Many websites suggest drinking a ton of water or taking a cold shower. Here's the subtle error: for some people, especially those with certain heart conditions, rapidly increasing fluid volume can temporarily increase the heart's workload. And a cold shower can cause blood vessels in the skin to constrict further, potentially raising pressure for some. The safest first interventions are always postural and respiratory.
Step-by-Step: What to Do Right Now (The Safe Way)
Follow these steps in order. They are designed to be safe for almost anyone and address the root cause – stress – without introducing new risks.
Step 1: Stop and Sit Down (The Right Way)
Immediately stop whatever you're doing. If you're arguing, stop. If you're rushing, stop. Find a quiet place to sit. But don't just slump on the couch.
The optimal position is a semi-reclined seated position. Sit in a comfortable chair or propped up in bed. The goal is to have your legs uncrossed and supported, slightly below the level of your heart. This reduces the gravitational pull on blood in your legs and can ease the workload on your heart. Sitting upright but slightly reclined is better than lying completely flat for a sudden spike.
Take off any tight clothing around your neck or waist.
Step 2: Practice Deep Breathing – The 4-7-8 Method
This isn't just “take a deep breath.” You need a structured technique to activate your parasympathetic nervous system (the “rest and digest” system). The 4-7-8 method is backed by evidence and is incredibly simple.
- Close your mouth and inhale quietly through your nose for a count of 4.
- Hold your breath for a count of 7.
- Exhale completely through your mouth, making a whoosh sound, for a count of 8.
Repeat this cycle four times. Focus only on the counts and the sound of your breath. This forces your heart rate to slow and signals your blood vessels to relax. Do this for at least 5 minutes. I've seen patients shave 15 points off their systolic reading just with this, measured 10 minutes apart.
Step 3: Hydrate Wisely
Now, drink a glass of room-temperature water. Not a gallon, not a sports drink, just 8-12 ounces of plain water. If you are dehydrated, your blood volume is lower and your body may be compensating by constricting vessels. Mild rehydration can help. Avoid ice-cold water, as the shock can sometimes trigger a brief constriction response.
Step 4: Consider a Quick Dietary Fix (If Appropriate)
This step has a big caveat. If your spike is due to sudden, high sodium intake (you just ate a very salty meal), consuming a potassium-rich food can help counterbalance fluid retention. But only if you have no kidney problems and are not on potassium-sparing medications. If you're unsure, skip this step.
A safe option is to eat a small banana or a handful of washed, no-salt-added sunflower seeds. The potassium helps your kidneys excrete more sodium. Don't go overboard. This is a minor supportive measure, not a primary treatment.
After completing these steps, wait 30-60 minutes in your calm, seated position. Then, recheck your blood pressure. Use proper technique: arm supported at heart level, feet flat, no talking.
Critical Warning Signs: When Home Treatment is NOT Enough
This is the most important section. Home treatment stops immediately if you experience any of the following. These are signs of a hypertensive emergency, where high pressure is causing direct damage to your organs. According to guidelines from the American Heart Association, this requires immediate medical care.
- Chest pain or severe pressure (could be a heart attack).
- Severe shortness of breath (could be heart failure).
- Severe headache, confusion, blurred vision, or difficulty speaking (could be a stroke or brain swelling).
- Nausea, vomiting, or severe anxiety that feels different from normal.
- Seizures or loss of consciousness.
- If your blood pressure is consistently above 180/120 and you feel unwell, even without the symptoms above.
In these cases, do not drive yourself. Call emergency services (911 or your local equivalent). Tell them you are experiencing a hypertensive crisis.
Common Mistakes That Can Make Things Worse
In a panic, people do irrational things. Here’s what to absolutely avoid.
Taking an Extra Dose of Your Blood Pressure Medication. This is potentially the most dangerous mistake. Medications work over hours. Doubling up won't fix an immediate spike but can cause your pressure to plummet dangerously low later, leading to falls, fainting, or kidney damage.
Drinking Alcohol or Caffeine. “A drink to calm your nerves” will dilate and then constrict blood vessels and is a terrible idea. Caffeine is a stimulant and will directly counteract your calming efforts.
Taking Over-the-Counter Painkillers (NSAIDs). Ibuprofen (Advil, Motrin), naproxen (Aleve), and even high-dose aspirin can cause your kidneys to retain sodium and water, raising blood pressure. They also reduce the effectiveness of many common blood pressure drugs. If you have a headache from the hypertension, taking these can create a vicious cycle.
Smoking or Vaping. Nicotine is a powerful vasoconstrictor. It will directly raise your blood pressure within minutes.
Vigorous Exercise. While regular exercise is key for long-term control, trying to “work off” a sudden spike puts massive strain on your cardiovascular system.
Long-Term Strategies to Prevent Future Spikes
An immediate crisis is a warning sign. The real work happens every day. The Centers for Disease Control and Prevention (CDC) emphasizes lifestyle modification as first-line therapy.
Know Your Triggers: Keep a simple log for a week. Note your pressure, what you ate, your stress level, and activity. You might find your spikes happen after salty lunches, during late-afternoon work stress, or when you skip your morning walk.
The DASH Diet Isn't Just a Fad: The Dietary Approaches to Stop Hypertension (DASH) eating plan is one of the most studied and effective non-drug approaches. It’s not about deprivation, but about adding more fruits, vegetables, whole grains, and lean proteins while reducing sodium. A common pitfall is only focusing on the “don'ts” (no salt) and missing the “dos” (more potassium, magnesium, calcium).
Consistency with Medication: If you are prescribed medication, take it at the same time every day. Setting a phone alarm is non-negotiable. The number one reason for “uncontrolled” hypertension in patients on medication is simply missing doses.
Manage Stress Proactively: The 4-7-8 breathing you learned for emergencies? Do it for 2 minutes, twice a day, every day. It trains your nervous system to be more resilient. Consider mindfulness apps or short daily walks in nature.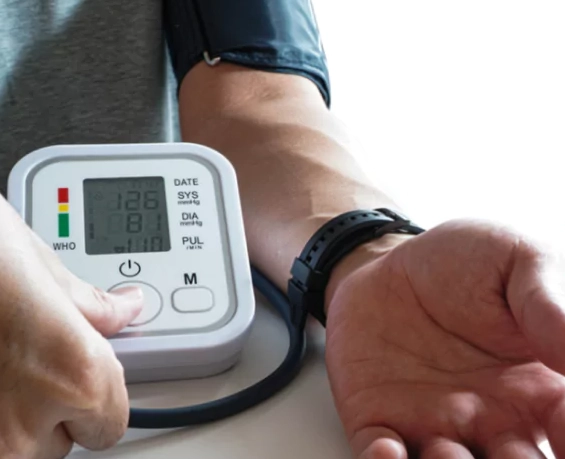
Your Questions Answered: Hypertension Emergency FAQ
My head is pounding. Can I take ibuprofen or aspirin?
What if I forgot to take my regular blood pressure medication today?
I feel anxious, which is making it worse. How can I calm down quickly?
Are there any foods I should eat right now to lower my BP?
How often should I recheck my pressure during a spike?
The key takeaway is that immediate treatment for high blood pressure at home is about intelligent, safe crisis management, not DIY medicine. It's about creating a window of stability to make a rational decision. By mastering these steps, you move from a place of fear to a place of control. Use this knowledge wisely, listen to your body's warning signs, and always partner with your healthcare provider for long-term management. Your health is worth that calm, informed approach.




Leave a comment