You feel it first – a pounding headache right behind your eyes, maybe some dizziness, a bit of shortness of breath. You check your blood pressure monitor, and the numbers stare back at you: 180/110. Your heart starts racing even faster. This is the moment most people panic, and that panic makes everything worse. Knowing what constitutes true first aid for high blood pressure isn't about magical cures; it's about a series of deliberate, calm actions to lower your risk of stroke, heart attack, or organ damage while you decide if you need an ambulance. Let's cut through the noise and get to what actually works.
What’s Inside: Your Quick Guide
- Is This a Real Emergency? Understanding the Numbers
- The 5 Immediate First Aid Steps (Before You Call Anyone)
- The Red Flags: When to Call 911 Immediately
- The Critical Medication Mistake Almost Everyone Makes
- What to Do After the Spike: Beyond the Emergency
- Your Top Questions on BP First Aid, Answered
Is This a Real Emergency? Understanding the Numbers
Not every high reading is a 911 call, but knowing the difference is crucial. Doctors categorize severe spikes into two groups, and confusing them can lead to bad decisions.
| Condition | Blood Pressure Reading | Key Symptom Difference | Immediate Goal |
|---|---|---|---|
| Hypertensive Urgency | Top number (systolic) > 180 and/or Bottom number (diastolic) > 120 | NO signs of acute organ damage. You might feel awful (headache, anxiety), but your brain, kidneys, eyes are not under immediate attack. | Lower BP safely over hours to days with medical guidance. This is where home first aid is most applicable. |
| Hypertensive Emergency | Same high readings (e.g., 200/130) | YES – there are signs of acute organ damage. This includes chest pain, severe headache with confusion, shortness of breath, seizures, blurred vision. | Immediate hospitalization to lower BP in minutes to hours with IV medication. This is a 911 situation. |
Most of the time, when people search for "first aid for high blood pressure," they're likely in or fearing a Hypertensive Urgency scenario. The goal isn't to crash your BP to 110/70 in ten minutes—that's dangerous. The goal is to reduce it gradually and prevent it from tipping into a full-blown emergency.
The 5 Immediate First Aid Steps (Before You Call Anyone)
Here’s your action plan. Do these in order. I’ve seen too many patients skip to step 5 in a panic, which often backfires.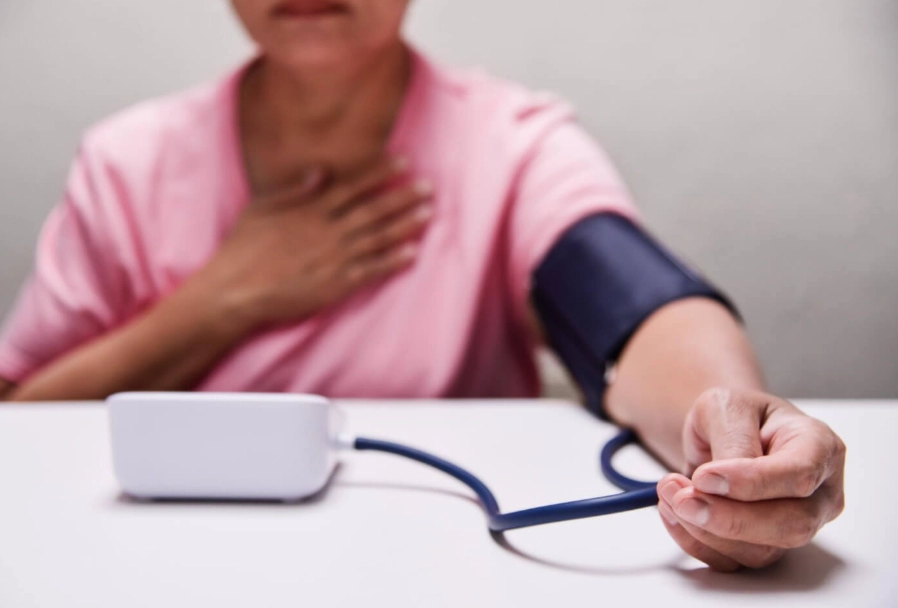
Step 1: Stop and Sit Down
This sounds too simple, but it's non-negotiable. If you're arguing, walking around, or trying to "power through," stop. Go to a quiet room and sit in a comfortable chair. Don't lie flat unless you feel faint; sitting upright is better for breathing. The physical act of stopping signals your nervous system to start downshifting.
Step 2: Practice the 4-7-8 Breathing Technique
Forget just "taking deep breaths." Use a structured method that forces your vagus nerve to engage. Here’s how: Inhale quietly through your nose for a count of 4. Hold your breath for a count of 7. Exhale completely through your mouth, making a whoosh sound, for a count of 8. Repeat this cycle 4-5 times. This is more effective than generic advice because the extended exhale is key to activating the parasympathetic (calming) nervous system.
Why This Works: Panic causes shallow chest breathing, which increases heart rate and BP. The 4-7-8 technique switches you to diaphragmatic breathing, directly lowering your sympathetic "fight or flight" response. It’s a physiological lever you can pull.
Step 3: Create a Calm Environment
Turn off loud TVs, harsh lights, and stressful conversations. If possible, dim the lights. Don’t start scrolling through your phone looking up scary complications—that’s mental gasoline on the fire. The aim is sensory deprivation from stressors.
Step 4: Take Your Medication Correctly (If Prescribed)
If you have "as-needed" medication like Clonidine or Labetalol, take it as your doctor instructed. Here’s the critical mistake: Do NOT take an extra dose of your regular long-term medication (like your morning Lisinopril or Amlodipine). These are not designed for rapid correction and can lead to unpredictable, sometimes dangerous drops in BP hours later. If you're unsure, this is what you call your doctor or pharmacist about.
Step 5: Re-check and Re-assess in 30-60 Minutes
After completing steps 1-4, wait. Don't re-check your BP every two minutes; the anxiety of the cuff inflating can keep it elevated. Set a timer for 30-60 minutes. Then, calmly re-check. A modest drop (even 10-15 points in the top number) is a good sign that your first aid is working and you may not be in an immediate emergency.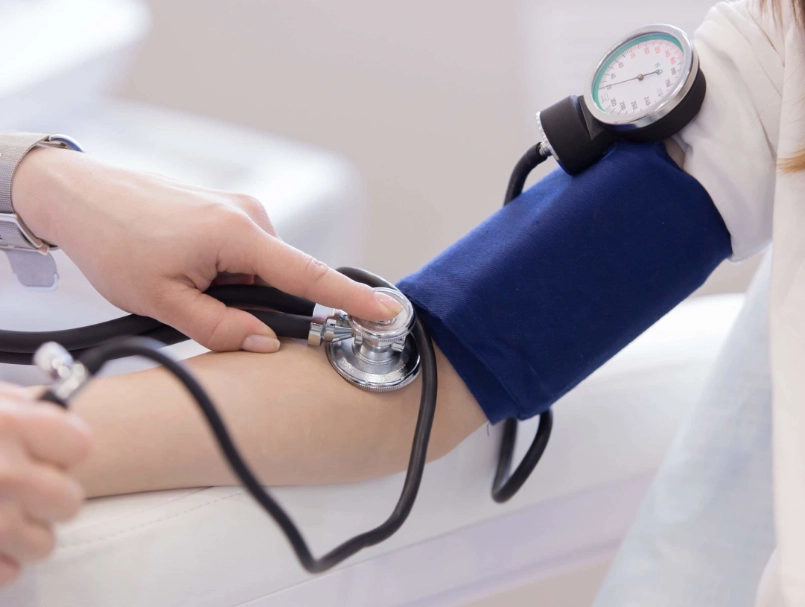
The Red Flags: When to Call 911 Immediately
First aid is for urgent situations. These symptoms mean the situation is now an emergency. Do not drive yourself. Call 911.
- Chest pain, pressure, or a squeezing sensation. This is heart attack territory.
- Severe headache, confusion, blurred vision, or difficulty speaking. These are potential stroke signs.
- Shortness of breath or coughing up pink, frothy mucus. This suggests fluid in the lungs (pulmonary edema).
- Seizures or loss of consciousness.
- Severe nausea and vomiting you can't control.

If you have any of these symptoms alongside a very high BP reading, your first aid is the phone. Call 911. Tell them, "I have extremely high blood pressure and [mention the symptom, e.g., chest pain]." This gets you the right response faster.
The Critical Medication Mistake Almost Everyone Makes
Let me share an observation from years in clinical practice. The most common, well-intentioned error I see is the "double-up" panic move. Someone with a reading of 190/115 who normally takes Amlodipine in the morning will take a second pill in the evening, thinking "more must be better."
It's not. These medications have a long, cumulative effect. Doubling up can cause your BP to plummet dangerously 6-12 hours later, leading tofalls, fainting, and insufficient blood flow to your brain and kidneys. The correct action is to take your next scheduled dose at the normal time, unless your doctor has given you explicit, different instructions for a crisis.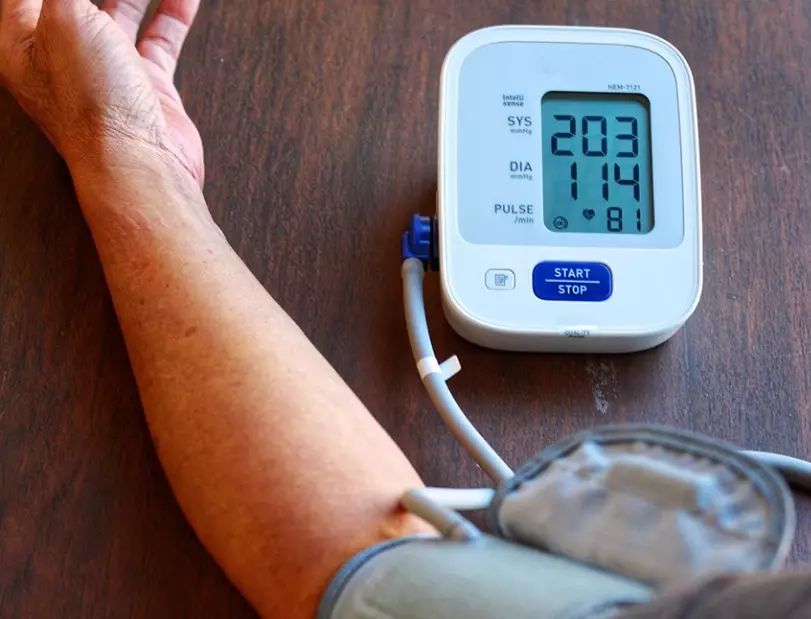
What to Do After the Spike: Beyond the Emergency
Once the acute spike is over, the real work begins. An urgent episode is a glaring warning sign that your long-term management plan isn't working.
- Schedule a Doctor's Appointment within 24-48 hours. Don't wait for your next routine checkup in 6 months. You need a plan adjustment.
- Audit Your Triggers: Was it an intense argument? Skipped medication for two days? A weekend of very salty food? Extreme stress at work? Pinpointing the trigger is your best clue for prevention.
- Consider a 24-hour BP Monitor: Ask your doctor about this. A single high reading at home might be an anomaly. A 24-hour monitor shows the full picture—how your BP behaves during sleep, work, and meals.
Long-term control is about consistency: taking meds as prescribed, reducing sodium (aim for under 1500mg daily), regular moderate exercise (like brisk walking), and managing stress with daily practices, not just in a crisis.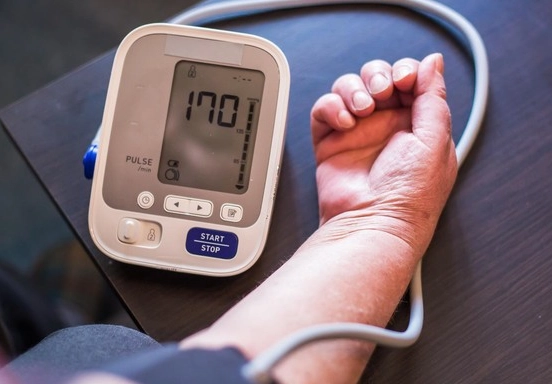
Your Top Questions on BP First Aid, Answered
I felt dizzy and my reading was high, but it went down after resting. Was that an emergency?
Are there any foods or drinks that can act as quick first aid for high blood pressure?
My home monitor shows a high reading, but I feel fine. Should I still do the first aid steps?
How accurate are home blood pressure monitors, and could mine be wrong?
I'm terrified of having a stroke every time my BP goes up. How do I manage this anxiety?
The bottom line is this: Effective first aid for high blood pressure is less about a secret trick and more about a disciplined, calm response. It's knowing when to act at home and when to hand it over to the professionals. By having this plan, you replace panic with purpose, which might be the most important step of all.


Leave a comment