If you're a woman feeling constantly drained, battling unexplained weight shifts, or riding an emotional rollercoaster, your thyroid might be the silent culprit. I've spent years writing about women's health, and the thyroid is one of the most misunderstood, yet critical, pieces of the puzzle. It's not just about "being tired" – it's a complex gland that influences everything from your heart rate to your mood. The challenge? Thyroid symptoms in women often masquerade as everyday stress or aging, leading to years of misdiagnosis. This guide cuts through the noise. We'll move beyond basic lists to explore how thyroid disease feels for women, the precise steps for getting an accurate diagnosis, and what treatment actually involves, from medication nuances to lifestyle adjustments that most doctors gloss over.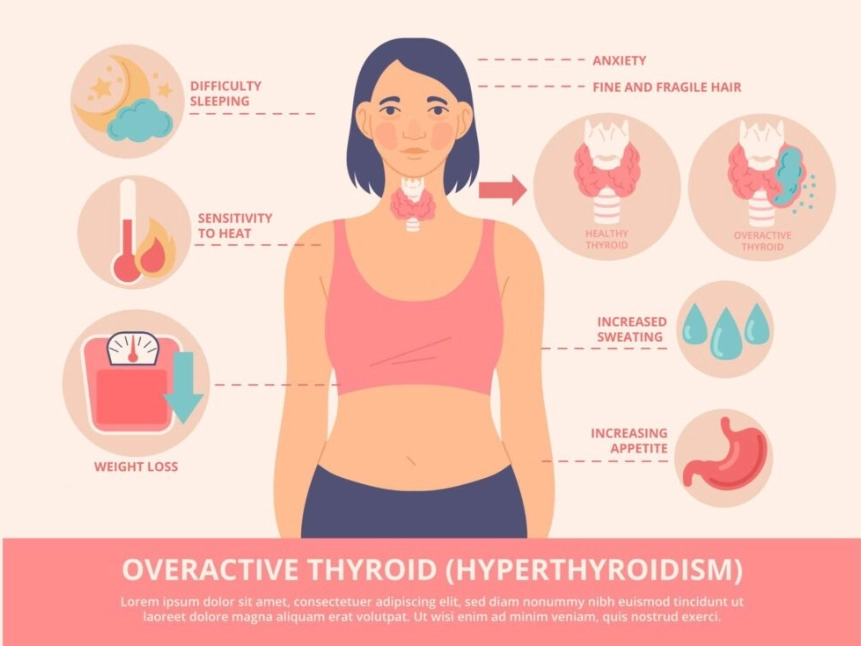
Your Quick Guide to Thyroid Health
Understanding Your Thyroid: The Body's Thermostat
Think of your thyroid gland, that butterfly-shaped organ in your neck, as your body's master metabolic controller. It produces hormones—primarily T4 (thyroxine) and T3 (triiodothyronine)—that set the pace for how every cell uses energy. When it's off, your whole system is off.
The two main dysfunctions are:
- Hypothyroidism (Underactive Thyroid): The gland doesn't produce enough hormones. Everything slows down. Metabolism, digestion, even your thought processes. Hashimoto's thyroiditis, an autoimmune disorder where your body attacks the thyroid, is the most common cause in women.
- Hyperthyroidism (Overactive Thyroid): The gland goes into overdrive, flooding your system with hormones. Your body races. Graves' disease, another autoimmune condition, is a frequent culprit here.
Why are women, particularly, in the crosshairs? The American Thyroid Association notes that women are 5 to 8 times more likely than men to have thyroid problems. The link isn't fully understood, but it's heavily tied to our complex hormonal ecosystem. Estrogen and progesterone fluctuations during puberty, pregnancy, perimenopause, and menopause seem to interact with thyroid function and immune response in ways that make us more susceptible.
A Personal Note: I've spoken to countless women who were told their symptoms were "just anxiety" or "part of being a busy mom." One woman, Sarah, spent a decade treating depression before a new doctor thought to check her TSH. Her level was 8.2 mIU/L (well above the ideal range). Starting thyroid hormone replacement didn't just fix her energy; it cleared a brain fog she didn't even fully realize she had. That's the insidious part.
Thyroid Symptoms in Women: Beyond Fatigue and Weight Gain
Yes, fatigue and weight changes are hallmarks. But focusing solely on them misses the bigger, messier picture. Thyroid symptoms in women are a full-body experience, often mimicking other conditions. Here’s a breakdown that goes deeper.
The Subtle Signs of an Underactive Thyroid (Hypothyroidism)
It’s not just moving slower. It’s feeling cold in a warm room, wearing socks to bed in July. It’s your hair thinning not just on your head, but the outer third of your eyebrows vanishing. It’s constipation that doesn't respond to diet changes, and a hoarse voice you attribute to allergies. Skin becomes dry and pale, almost waxy. Periods get heavier, longer, and more painful. You might feel a vague swelling in your neck or a constant need to clear your throat. The mental fog is real—forgetfulness, struggling to find words, a lack of motivation that feels like a character flaw rather than a chemical one.
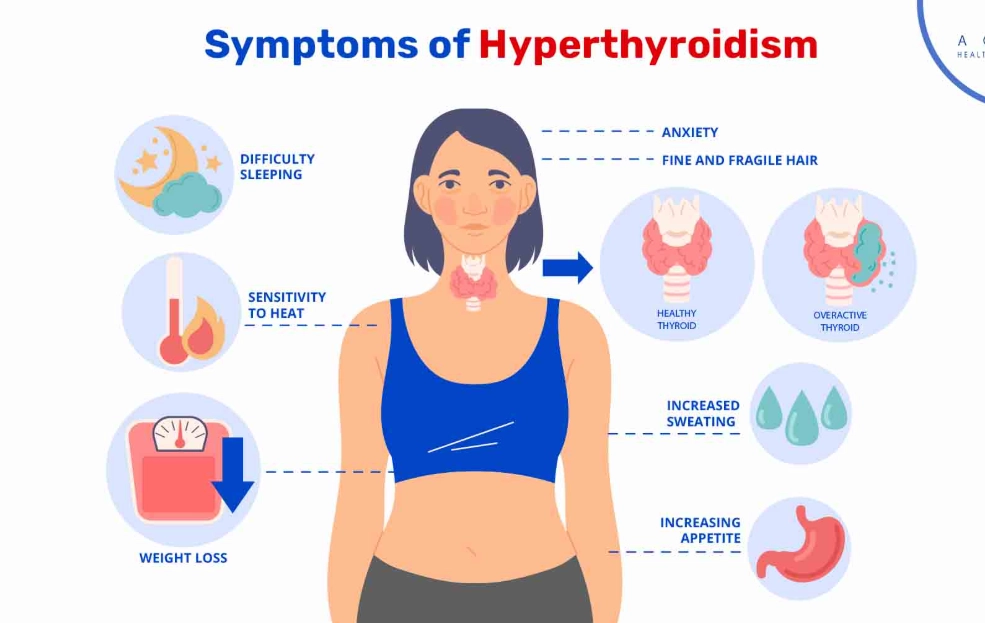
The Frenetic Signs of an Overactive Thyroid (Hyperthyroidism)
This isn't productive energy. It's a jittery, anxious, can't-sit-still feeling. Your heart might pound or skip beats (palpitations). You're hot and sweaty when others are comfortable. Despite eating more, you lose weight without trying—a red flag many dismiss. Hands may develop a fine tremor. Periods become light or stop altogether. Sleep is elusive despite exhaustion. A telltale sign can be bulging or gritty, irritated eyes, often associated with Graves' disease.
| Symptom Area | Hypothyroidism (Underactive) | Hyperthyroidism (Overactive) |
|---|---|---|
| Energy & Mood | Profound fatigue, depression, brain fog, low motivation | Nervousness, anxiety, irritability, restlessness |
| Metabolism & Weight | Unexplained weight gain, difficulty losing weight | Unintentional weight loss despite increased appetite |
| Physical Sensations | Cold intolerance, dry skin, muscle aches, constipation | Heat intolerance, excessive sweating, diarrhea, tremors |
| Reproductive Health | Heavy, irregular periods, fertility issues | Light, infrequent periods, menstrual irregularities |
| Appearance | Puffy face, dry/thinning hair, loss of outer eyebrows | Thinning skin, fine hair, possible bulging eyes (Graves') |
| Cardiac | Slow heart rate (bradycardia) | Rapid or irregular heartbeat (palpitations, atrial fibrillation) |
See how many overlap with stress, perimenopause, or just life? That's why testing is non-negotiable.
How is Thyroid Disease Diagnosed in Women?
You can't treat what you don't measure correctly. Here’s the step-by-step process, including the pitfalls.
Step 1: The Blood Test Panel. Don't settle for just TSH (Thyroid Stimulating Hormone). A full panel is crucial. This includes:
- TSH: The primary screening tool. High TSH usually indicates hypothyroidism; low TSH suggests hyperthyroidism.
- Free T4 & Free T3: These measure the actual thyroid hormones circulating and available for your cells to use.
- Thyroid Antibodies (TPO & TgAb): This tests for autoimmune activity (Hashimoto's or Graves'). This is the key to understanding the cause.
The Lab Range Trap: Many labs use wide "normal" reference ranges (often 0.4 – 4.0 mIU/L for TSH). However, most functional medicine and progressive endocrinology experts argue the optimal range for feeling well is much narrower, often between 1.0 and 2.5 mIU/L. A TSH of 3.8 might be "in range" but leave you feeling terrible. This is a major point of contention and a reason many women feel dismissed.
Step 2: The Physical Exam. Your doctor should feel (palpate) your neck for goiter (enlargement) or nodules.
Step 3: Imaging (if needed). An ultrasound can assess the gland's structure, identify nodules, and check for inflammation patterns typical of Hashimoto's.
Bring a detailed symptom journal to your appointment. Dates, patterns, severity. It turns subjective feelings into clinical data.
What are the Treatment Options for Thyroid Conditions?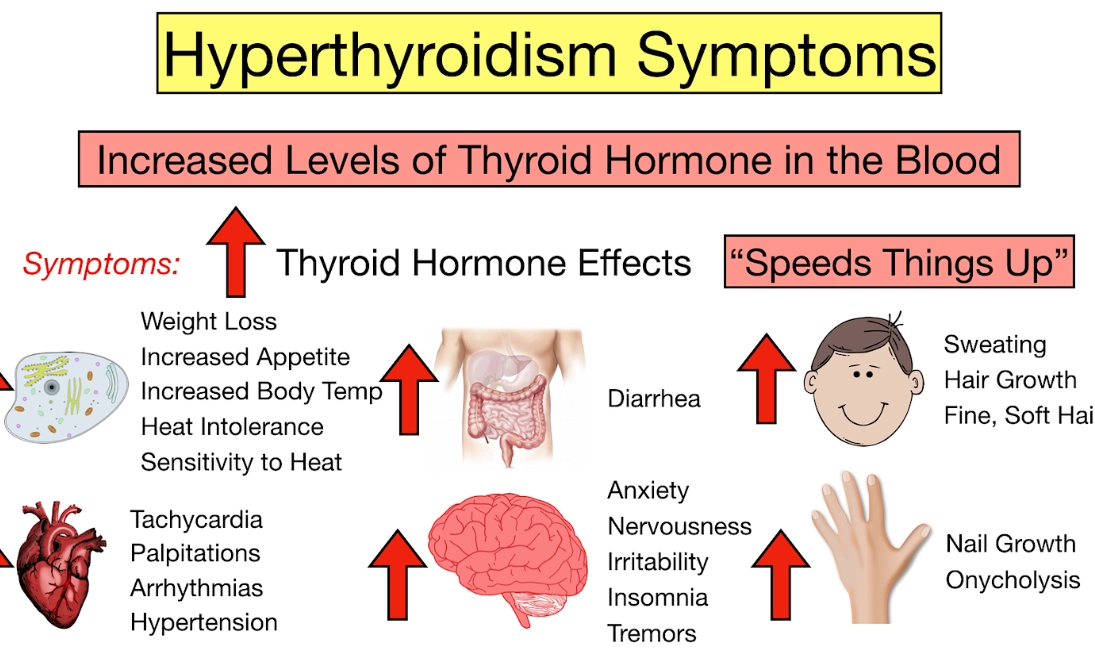
Treatment isn't one-size-fits-all. It's a partnership with your doctor, often requiring fine-tuning.
Treatment for Hypothyroidism
The cornerstone is thyroid hormone replacement therapy.
- Levothyroxine (Synthroid, Levoxyl, Tirosint, Unithroid): This is synthetic T4. Your body converts it to the active T3. It's the standard first-line treatment. The key is consistency: take it on an empty stomach with water only, at least 30-60 minutes before food, coffee, or other medications (especially calcium or iron supplements).
- Natural Desiccated Thyroid (NDT) (Armour Thyroid, NP Thyroid): Derived from porcine thyroid glands, it contains both T4 and T3. Some patients report feeling better on NDT, especially if they have a conversion issue (trouble turning T4 into T3). However, its hormone ratios are fixed and not FDA-approved to the same degree as levothyroxine. It's a conversation to have with an open-minded endocrinologist.
- Liothyronine (Cytomel): This is synthetic T3. Sometimes added to levothyroxine if T3 levels remain low.
Adjusting the dose is normal. It can take 6-8 weeks for a new dose to stabilize in your system before re-testing.
Treatment for Hyperthyroidism
The goal is to reduce hormone production.
- Anti-thyroid Medications (Methimazole, Propylthiouracil/PTU): These drugs block the thyroid's ability to make hormones. They are often used as a first step, especially for Graves' disease, to achieve a "euthyroid" (normal) state. Treatment can last 12-18 months or longer.
- Radioactive Iodine (RAI) Therapy: You swallow a radioactive iodine pill that destroys overactive thyroid cells. This often leads to permanent hypothyroidism, requiring lifelong thyroid hormone replacement. It's a definitive treatment but changes your thyroid status.
- Thyroid Surgery (Thyroidectomy): Removing part or all of the thyroid gland. Considered for large goiters, suspected cancer, or if other treatments aren't suitable or have failed. Like RAI, it usually results in hypothyroidism.
Beta-blockers (like propranolol) are often prescribed short-term to manage rapid heart rate, tremors, and anxiety while the primary treatment takes effect.
Living Well with a Thyroid Condition
Medication is the foundation, but lifestyle is the framework that holds everything together. This is where you take control.
Diet & Nutrients: There's no universal "thyroid diet," but some principles help. Ensure adequate selenium (Brazil nuts, tuna) and zinc (pumpkin seeds, lentils) which support hormone conversion. Iodine is tricky: deficiency causes problems, but excess can worsen autoimmune thyroiditis. Don't mega-dose without testing. For Hashimoto's, some find reducing gluten and dairy reduces inflammatory symptoms, though evidence is mixed. Cruciferous vegetables (broccoli, kale) are fine cooked; raw in extreme amounts might interfere with iodine uptake, but you'd have to eat a truckload.
Stress Management: Chronic stress raises cortisol, which can disrupt thyroid hormone conversion and immune function. This isn't fluff. Find what works: daily walks, meditation, yoga, or simply setting boundaries.
Sleep & Routine: Prioritize 7-9 hours of quality sleep. A consistent daily routine helps regulate your circadian rhythm, which influences thyroid function.
Exercise: Do it, but listen to your body. With hypothyroidism, intense cardio might wipe you out. Focus on gentle strength training, walking, swimming, or yoga to build metabolism-supporting muscle without overtaxing your system.
Track your symptoms, energy levels, and medication timing in a simple app or notebook. It provides invaluable data for your next doctor's visit.
Your Thyroid Questions, Answered
 Can thyroid issues affect pregnancy and fertility?
Can thyroid issues affect pregnancy and fertility?Managing thyroid health is a journey, not a one-time fix. It requires becoming an expert on your own body, partnering with a responsive healthcare provider, and making consistent, supportive lifestyle choices. The goal isn't just a "normal" lab result—it's feeling like yourself again.





Leave a comment