Let's cut straight to it. There is no single "best" infertility treatment for everyone. I know that's not the simple answer you might be hoping for, but it's the honest truth after seeing countless couples navigate this. The "best" treatment is the one that's tailored to your specific diagnosis, your age, your medical history, your emotional resilience, and yes, your budget. Asking for the best is really asking, "What's the most effective path for someone in my exact situation?" This guide will help you answer that.
We'll move from understanding why you're struggling to conceive, through the maze of treatment options, all the way to the practical and emotional realities of the journey. Think of it as a roadmap, not a prescription.
Your Quick Navigation Guide
- How Infertility is Diagnosed: The First Crucial Step
- What is the Best Treatment for Infertility? (Spoiler: It Depends)
- A Detailed Look at Common Fertility Treatments
- Beyond Medicine: The Critical Role of Lifestyle and Support
- How to Choose the Right Fertility Clinic and Specialist?
- Your Fertility Treatment Questions Answered
How Infertility is Diagnosed: The First Crucial Step
Jumping straight to IVF because it's "the best" is like trying to fix a car without opening the hood. You might get lucky, but you'll probably waste a ton of time and money. A proper diagnosis is non-negotiable.
The standard definition of infertility is trying to conceive for 12 months without success if you're under 35, or for 6 months if you're 35 or older. But if you have irregular cycles, known conditions like PCOS or endometriosis, or a history of pelvic surgery, don't wait. See a specialist sooner.
The diagnostic workup is a partnership. It typically involves both partners from day one.
Standard Fertility Workup Checklist
For the female partner: This starts with a detailed history and physical. Key tests include a Day 3 FSH and AMH to check ovarian reserve (egg supply), an ultrasound to look at the ovaries and uterus, and a hysterosalpingogram (HSG) – an X-ray dye test to see if the fallopian tubes are open. Tracking ovulation with urine kits or blood tests is also standard.
For the male partner: It begins and often ends with a semen analysis. This isn't a test of masculinity; it's a basic, critical piece of data. It checks sperm count, movement (motility), and shape (morphology). If it's abnormal, it's repeated. If it's still abnormal, the next step is usually a visit to a urologist who specializes in male fertility.
A surprising number of cases have a combination of factors from both partners.
What is the Best Treatment for Infertility? (Spoiler: It Depends)
Okay, now we can talk about treatments. The "best" one is the least invasive, most effective option that addresses your specific problem. Treatments are a staircase, not a random list.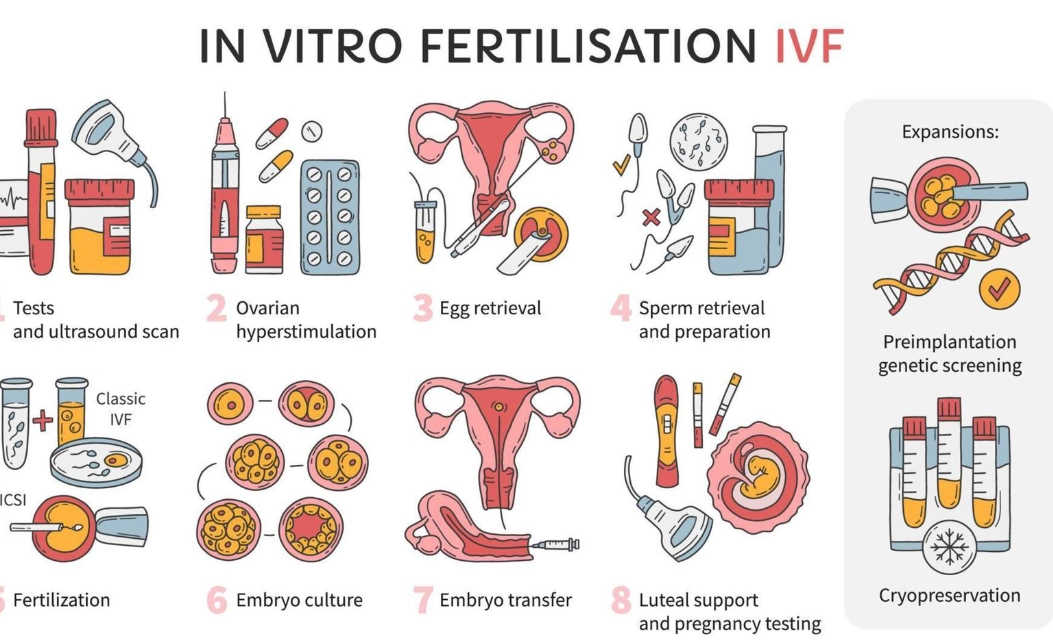
Here’s the general progression most reproductive endocrinologists follow:
- Lifestyle Optimization & Timed Intercourse: For very mild issues, this might be enough. It involves confirming ovulation and timing sex correctly.
- Ovulation Induction with Oral Medications: The first-line medical treatment for women who aren't ovulating regularly (like with PCOS). Clomiphene citrate or letrozole are common.
- Intrauterine Insemination (IUI): Often combined with ovulation-inducing drugs. Washed, concentrated sperm is placed directly into the uterus around ovulation. Good for mild male factor, cervical issues, or unexplained infertility.
- In Vitro Fertilization (IVF): The most powerful tool. Eggs are retrieved, fertilized with sperm in a lab, and resulting embryos are transferred into the uterus. This bypasses many problems (tube blockages, severe male factor).
A Detailed Look at Common Fertility Treatments
Let's break down the main players. This table gives you the big picture, but the devil is in the details—and the details are what your doctor is for.
| Treatment | How It Works | Best For | Typical Success Rate* (Per Cycle) | Key Considerations |
|---|---|---|---|---|
| Ovulation Induction (OI) (e.g., Clomid/Letrozole) |
Oral pills stimulate the ovaries to produce and release one or more eggs. | Women with irregular or absent ovulation (e.g., PCOS). | 10-20% pregnancy rate (with timed intercourse). | Risk of multiples (twins). Requires monitoring via ultrasound. Cheap compared to other treatments. |
| Intrauterine Insemination (IUI) | Sperm is washed and placed directly into the uterus at the time of ovulation. | Unexplained infertility, mild male factor, cervical issues, using donor sperm. | 10-20% pregnancy rate (higher when combined with OI drugs). | Still requires at least one open tube and decent sperm. Usually tried for 3-6 cycles before moving on. |
| In Vitro Fertilization (IVF) | Eggs retrieved, fertilized in lab, embryo(s) transferred to uterus. | Tubal blockages, severe male factor, endometriosis, advanced maternal age, failed IUI, genetic screening. | Varies widely by age. ~55% for women under 35; ~35% for women 38-40 (per embryo transfer). | High cost, physically and emotionally intense. Allows for genetic testing of embryos (PGT-A). |
| ICSI (Intracytoplasmic Sperm Injection) | A single sperm is injected directly into an egg during IVF. | Severe male factor infertility (very low count/poor motility), previous IVF fertilization failure. | Similar to standard IVF success rates for a given age group. | Now used in over 60% of IVF cycles in the U.S., sometimes even for non-male factor cases (a debated practice). |
| Fertility Preservation (Egg/Embryo Freezing) |
Eggs or embryos are frozen for future use. | Women delaying childbearing for medical (e.g., cancer) or personal reasons. | Success depends on age at freezing and number of eggs/embryos stored. | Not a treatment for current infertility, but a proactive strategy. Success is not guaranteed. |
*Success rates are highly clinic and patient-specific. Always ask a clinic for their SART (Society for Assisted Reproductive Technology) reported data, which is standardized. You can look up any U.S. clinic on the SART website.
IVF isn't one thing. It's a process with many decision points: what drugs for stimulation? How many embryos to transfer? Should we test the embryos genetically (PGT-A)? These choices dramatically impact success and risk. A 40-year-old transferring one untested embryo has different odds than a 30-year-old transferring one genetically screened embryo.
The Reality of Success Rates and "The Numbers Game"
People get obsessed with clinic success rates. It's important, but context is everything. A clinic with a 70% success rate might only accept young, healthy patients. Another with a 50% rate might take on complex cases. Look at the data for your age group.
More crucial than the clinic's overall rate is your personal prognosis. How many eggs do you typically produce? What's your embryo quality? Infertility treatment, especially IVF, can feel like a brutal numbers game. It often takes more than one cycle. Financially and emotionally planning for that possibility from the start is a form of self-care many regret not doing.
Beyond Medicine: The Critical Role of Lifestyle and Support
Doctors focus on the medical protocol. But the environment you create for that protocol matters. I'm not talking about miracle diets. I'm talking about foundational health.
Nutrition: Ditch the extreme cleanses. Focus on a balanced, anti-inflammatory diet—think Mediterranean. Enough protein, healthy fats, and plenty of vegetables. For men, antioxidants (like those found in berries and nuts) can support sperm health.
Weight: This is sensitive but real. Being significantly underweight or overweight can disrupt hormone balance and ovulation. Even a 5-10% reduction in body weight can restart ovulation in women with PCOS.
Stress: Don't let anyone tell you stress "caused" your infertility. That's cruel. But the process of treatment is profoundly stressful, and chronic stress doesn't help. Find what lowers your cortisol—yoga, therapy, walking, journaling. For me and my partner, it was setting a strict "no fertility talk" zone after 7 PM.
The Partner Dynamic: This journey can drive a wedge between you. You're both suffering, but often in different, silent ways. Go to appointments together when you can. Designate a point person for communicating with family. Consider couples therapy before you think you need it. It's maintenance, not repair.
How to Choose the Right Fertility Clinic and Specialist?
Your doctor and clinic are your teammates. You need to trust them.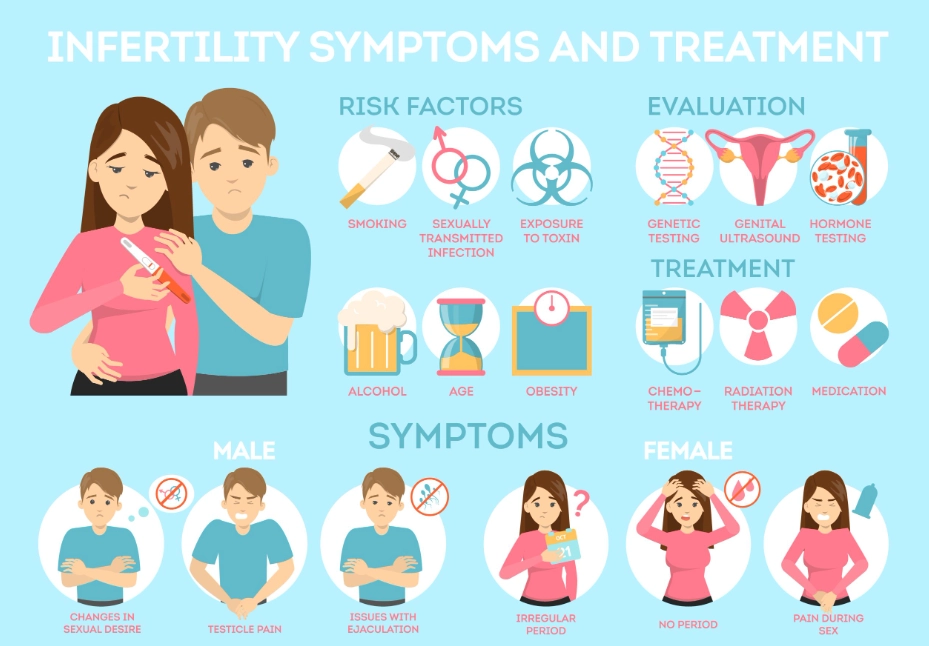
Don't just pick the one closest to you. Do the homework.
- Check the SART Data: As mentioned, this is your objective starting point. Look at live birth rates for your age group.
- Consultation Vibe: Did the doctor listen? Did they explain things clearly without rushing? Did they seem to have a plan, or did they offer a one-size-fits-all approach? Did they discuss costs openly?
- Clinic Logistics: How far is it? What are monitoring hours? Can you get someone on the phone in a crisis? The best medical protocol is useless if you can't adhere to it because the clinic is impossibly inconvenient.
- Financial Coordinator: Talk to them early. Get a detailed, written cost estimate. Understand what your insurance covers (if anything) and what the clinic's payment plans or refund programs are.
It's okay to get a second opinion. In fact, I encourage it if you have any doubts.
Your Fertility Treatment Questions Answered
 We've had two failed IVF cycles. The doctor says it's "bad luck" and to try again. How do we know when to stop or change course?
We've had two failed IVF cycles. The doctor says it's "bad luck" and to try again. How do we know when to stop or change course?




Leave a comment