Let's talk about something that feels incredibly lonely but is surprisingly common: female infertility. If you've been trying to conceive for a while without success, you're not alone. The journey can be confusing, emotionally draining, and filled with questions. I've spent years in this field, talking to countless women and couples, and one thing I've learned is that generic advice doesn't cut it. You need clear, specific information about what might be happening in your body.
Infertility isn't one single condition. It's a symptom, a signal that something in the complex process of ovulation, fertilization, or implantation isn't working as it should. The causes are varied, and they often overlap. A diagnosis of "unexplained infertility" is frustratingly common, but even then, there are usually clues if you know where to look.
This article breaks down the major causes of female infertility, not just as a medical textbook would, but with the practical insights and nuances you'd get from a long conversation with a specialist. We'll move beyond the basics into what these conditions actually feel like and what steps you can realistically take next.
Your Quick Guide to This Article
- When Your Body Doesn't Release an Egg: Ovulation Disorders
- Blocked Pathways and Unfriendly Environments: Fallopian Tube & Uterine Problems
- The Heavy Hitters: Endometriosis and PCOS
- Age, Lifestyle, and the Overlooked Factors
- How Do You Figure Out What's Wrong? The Diagnostic Path
- Your Top Questions Answered
When Your Body Doesn't Release an Egg: Ovulation Disorders
This is the single most common cause of female infertility, accounting for about 25% of cases. If you're not ovulating regularly, there's no egg for sperm to meet. It sounds simple, but the reasons behind anovulation (lack of ovulation) are complex.
Here's the big misconception: having a period doesn't always mean you ovulated. You can have what's called an anovulatory cycle, where you bleed but no egg was released. This is a key detail many women miss.
What Disrupts Ovulation?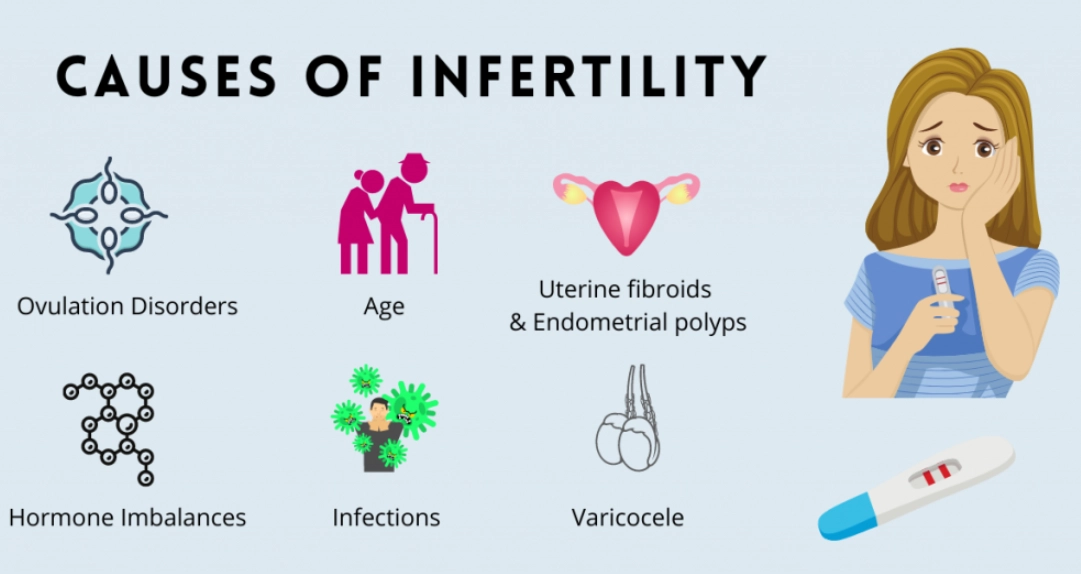
Your brain's hypothalamus and pituitary gland call the shots, telling your ovaries to get to work. Disrupt this communication, and everything stalls.
- Hypothalamic Dysfunction: Extreme stress, significant weight loss or low body weight, and excessive exercise can shut down the signal from the hypothalamus. Your body goes into "survival mode," prioritizing essential functions over reproduction. I've seen this in dedicated athletes and women under immense career pressure.
- Pituitary Issues: Conditions like hyperprolactinemia (high prolactin, the hormone that stimulates milk production) can suppress ovulation. Even a small, benign pituitary tumor can cause this. Thyroid disorders (both overactive and underactive) are also major culprits that throw the entire hormonal orchestra out of tune.
- Primary Ovarian Insufficiency (POI): Sometimes called premature ovarian failure, this is when the ovaries stop working normally before age 40. It's different from early menopause and can be intermittent, making it tricky to diagnose.
Blocked Pathways and Unfriendly Environments: Fallopian Tube & Uterine Problems
Imagine the perfect egg and the champion sperm, but they can't find each other because the meeting place is blocked or hostile. That's the realm of tubal and uterine factors.
Fallopian Tube Damage (Tubal Infertility)
The tubes are where fertilization happens. If they're blocked or scarred, the egg and sperm never meet. The main culprits?
- Pelvic Inflammatory Disease (PID): Often caused by untreated sexually transmitted infections like chlamydia or gonorrhea. The scary part? You can have a silent infection with no symptoms that still causes significant scarring. The CDC emphasizes regular STI screening as a preventive measure.
- Previous Surgery: Surgery in the pelvic area, like for appendicitis or ovarian cysts, can lead to adhesions (scar tissue) that bind the tubes.
- Ectopic Pregnancy: A past ectopic pregnancy in a tube often damages it, increasing the risk of another and reducing fertility in that tube.

Uterine or Cervical Abnormalities
This is about the "home" where the embryo needs to implant and grow.
- Uterine Fibroids: These non-cancerous growths are incredibly common. Whether they impact fertility depends entirely on their size and location. A small fibroid in the muscle wall might be harmless, while one that distorts the uterine cavity (submucosal) can act like an IUD, preventing implantation.
- Polyps: These small, benign growths on the uterine lining can create an inflammatory environment or simply get in the way.
- Scar Tissue (Asherman's Syndrome): Often from a past D&C procedure, especially after a miscarriage or delivery. The scar tissue replaces the normal lining.
- Cervical Issues: Rarely, the cervix produces mucus that is too thick for sperm to penetrate. Or, previous surgical procedures (like a LEEP or cone biopsy) can have altered cervical function.
The Heavy Hitters: Endometriosis and PCOS
These two conditions deserve their own spotlight because they're complex, often misunderstood, and major drivers of infertility.
| Condition | What It Is | How It Affects Fertility | A Key Insight Often Missed |
|---|---|---|---|
| Endometriosis | Tissue similar to the uterine lining grows outside the uterus (on ovaries, tubes, pelvic lining). | Creates inflammation, scar tissue (adhesions), and a toxic environment for eggs, sperm, and embryos. Can distort pelvic anatomy. | The severity of pain does NOT correlate with the severity of infertility. You can have debilitating pain with minimal impact on fertility, or silent endometriosis (no pain) that severely impacts egg quality and implantation. |
| Polycystic Ovary Syndrome (PCOS) | A metabolic and hormonal disorder characterized by irregular ovulation, high androgens (male hormones), and polycystic ovaries on ultrasound. | Irregular or absent ovulation is the primary issue. The hormonal imbalance can also affect egg quality and increase miscarriage risk. | It's not just about cysts. The root is insulin resistance in most cases. Managing blood sugar through diet and medication (like metformin) can be as crucial for fertility as drugs that induce ovulation. |
I can't stress this enough: if you have painful periods or highly irregular cycles, don't let anyone dismiss it as "just bad periods." Push for an evaluation. The American Society for Reproductive Medicine (ASRM) has excellent patient resources on both conditions.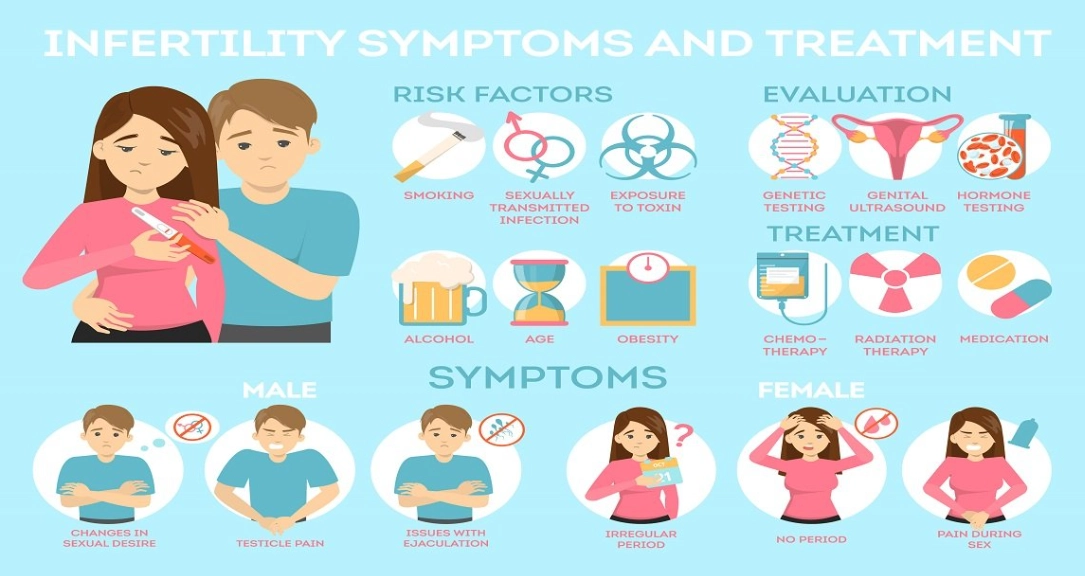
Age, Lifestyle, and the Overlooked Factors
We have to talk about age. It's not just a number here; it's the single most important factor for egg quality and quantity. A woman is born with all the eggs she'll ever have, and their quality declines gradually after 30, then more rapidly after 35. This isn't meant to scare you—it's biology. It means the chances of chromosomal abnormalities in eggs increase, leading to higher rates of miscarriage and lower success rates with treatment.
Lifestyle factors matter, but the internet gets the emphasis wrong.
- Weight: Both significantly low and high body weight can disrupt ovulation. Fat tissue produces estrogen. Too little body fat means not enough estrogen; too much can mean too much estrogen, confusing the hormonal feedback loop.
- Smoking: It ages your ovaries. Full stop. Smokers often reach menopause 1-4 years earlier.
- Alcohol & Caffeine: Heavy drinking is clearly detrimental. The data on moderate consumption and caffeine is murkier. My advice? If you're struggling, cutting back is a low-cost, zero-risk experiment you can run on yourself.
- The Mental Load: Chronic, severe stress can affect ovulation. But let's be clear: the stress of infertility is a result of the problem, not usually the cause. Telling someone to "just relax" is not only unhelpful, it's insulting.
How Do You Figure Out What's Wrong? The Diagnostic Path
The workup for infertility is like being a detective. You start with the most common, least invasive clues.
- Ovulation Confirmation: This is step one. Your doctor might recommend tracking your BBT, using OPKs, or checking a mid-luteal phase progesterone blood test (about 7 days after you think you ovulated).
- Ovarian Reserve Testing: This gives an idea of your egg supply. It involves blood tests (AMH, FSH, estradiol) on day 3 of your cycle and sometimes an antral follicle count via ultrasound.
- Checking the Plumbing: A hysterosalpingogram (HSG) is an X-ray test where dye is injected into the uterus to see if it spills out the ends of the tubes. It checks for blockages and uterine shape.
- Looking Inside: A laparoscopy is a surgical procedure where a camera is inserted into the abdomen. It's the gold standard for diagnosing endometriosis and checking for adhesions. It's more invasive, so it's not always the first test.
- Checking the Uterine Cavity: A saline infusion sonogram (SIS) or hysteroscopy uses fluid and ultrasound (or a camera) to look inside the uterus for polyps, fibroids, or scar tissue.
The goal isn't to do every test on everyone. A good specialist will tailor the path based on your history, age, and symptoms.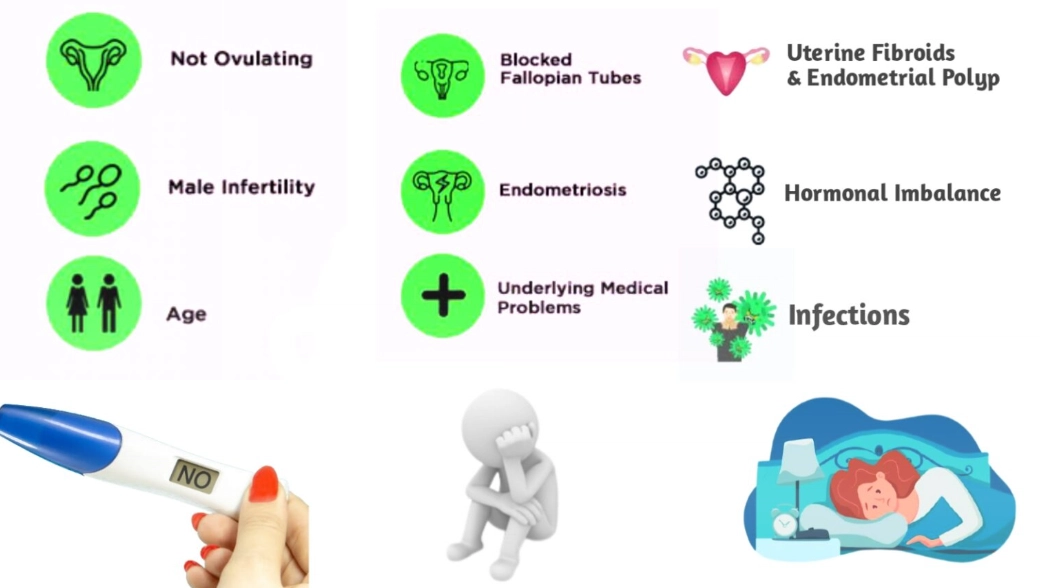
Your Top Questions Answered





Leave a comment