Let's cut to the chase. A sudden, severe spike in blood pressure can be terrifying. You're feeling awful, the numbers on your monitor look scary, and you're searching for a way to make it stop now. The most critical thing you need to understand is this: true "instant" lowering in a genuine emergency often requires emergency medical treatment. However, there are immediate, evidence-based actions you can take to help manage the situation while waiting for help or to address a severe but non-critical spike. This guide will walk you through exactly what defines a hypertensive emergency, the steps you can take right this minute, and the non-negotiable signs that mean you must call an ambulance.
Quick Navigation: What You'll Find Here
- What is a Hypertensive Emergency?
- How to Lower Blood Pressure Instantly in an Emergency: 5 Immediate Steps
- When You MUST Call 911 or Go to the ER
- What NOT to Do: Dangerous Home "Remedies"
- Beyond the Crisis: Long-Term Management to Prevent Another Emergency
- Your Emergency Blood Pressure Questions Answered
What is a Hypertensive Emergency?
Not every high reading is an emergency. This is a key point most articles gloss over. A hypertensive emergency (or hypertensive crisis) is defined by two factors:
- Extremely High Blood Pressure: Typically, a systolic (top number) reading over 180 mmHg and/or a diastolic (bottom number) reading over 120 mmHg.
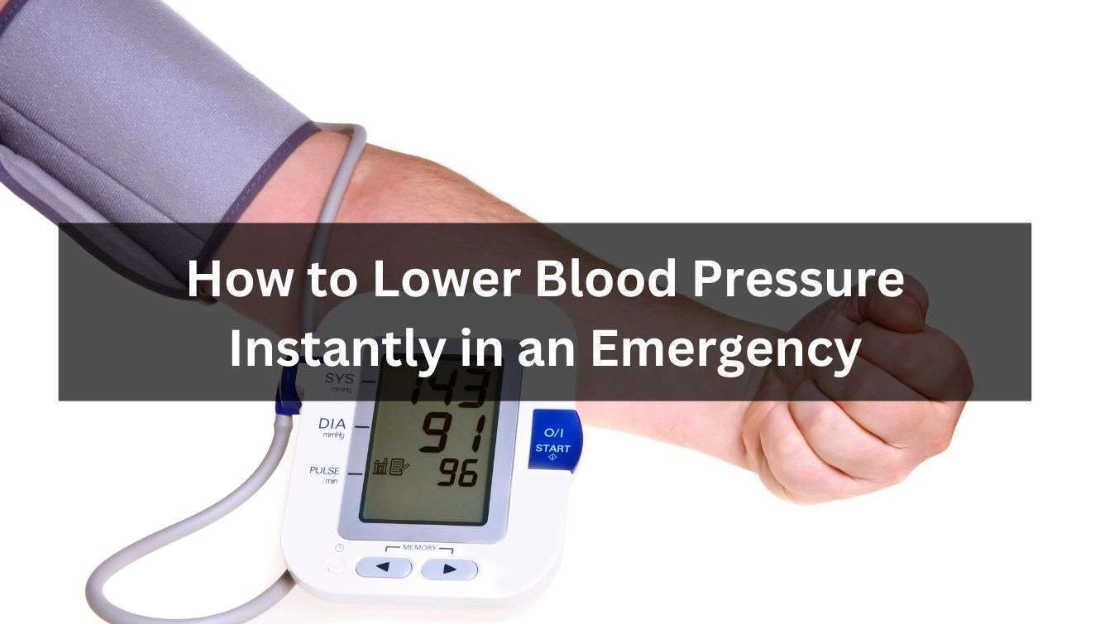
- Evidence of Acute Organ Damage: This is the crucial part. The high pressure is causing immediate harm. Symptoms might include chest pain (heart), shortness of breath (lungs), severe headache/vision changes/confusion (brain), or back pain (aorta).
If you have #1 but NOT #2, it's often called a "hypertensive urgency." It's still serious and needs prompt medical attention, usually within hours, but it may not require an ambulance if you can see a doctor immediately. The line is blurry, and erring on the side of caution is always safer.
| Situation | Typical BP Reading | Symptoms | Required Action |
|---|---|---|---|
| Hypertensive Emergency | >180/120 mmHg | Chest pain, severe headache, shortness of breath, vision changes, numbness, difficulty speaking, back pain. | CALL 911 IMMEDIATELY. This is life-threatening. |
| Hypertensive Urgency | >180/120 mmHg | Often none, or mild headache, anxiety. | Contact your doctor immediately or go to an urgent care/ER for evaluation within hours. Do not wait. |
| Stage 2 Hypertension | >140/90 mmHg | Usually none (it's the "silent killer"). | Schedule a prompt appointment with your doctor to adjust your long-term management plan. |
How to Lower Blood Pressure Instantly in an Emergency: 5 Immediate Steps
If you are experiencing a severe spike, follow these steps in order. Their goal is to reduce stress on your cardiovascular system while you seek or await professional care.
1. Sit Down and Breathe Deeply (The 4-7-8 Method)
Stop whatever you're doing. Sit in a comfortable chair with your back supported. Place your feet flat on the floor. Do not lie down flat unless you feel faint.
Now, breathe. Forget "just take deep breaths." Use the 4-7-8 technique: Inhale quietly through your nose for a count of 4. Hold your breath for a count of 7. Exhale completely through your mouth, making a whoosh sound, for a count of 8. Repeat this cycle 4-5 times. This activates your parasympathetic nervous system, which directly counters the stress response that's elevating your BP.
2. Create a Calm Environment
Turn off loud music or TV. Dim bright lights. Ask others to give you quiet space. If you were in an argument or stressful situation, physically remove yourself from it. This isn't about being rude; it's a medical necessity. The goal is to reduce sensory and emotional input that's fueling the crisis.
3. Do NOT Drink Alcohol, Smoke, or Have Caffeine
This seems obvious, but in a panic, people sometimes reach for a cigarette or a drink to "calm their nerves." These are vasoconstrictors—they tighten your blood vessels and will make your blood pressure worse. Drink a small glass of cool water instead. Dehydration can sometimes contribute to higher readings.
4. Take Your Prescribed Medication (If Directed by a Doctor)
This is a major point of confusion. Only take extra or different doses of your blood pressure medication if you have a specific, pre-arranged plan with your cardiologist for such situations. Some patients are prescribed a fast-acting medication like labetalol or captopril to take in case of a severe spike. If you don't have such a plan, do not experiment. Taking too much can cause a dangerous sudden drop.
5. Monitor and Record
If you can do so calmly, take your blood pressure after 10-15 minutes of following the steps above. Write down the time and the reading. This information is gold for the medical professionals who will be treating you. It shows the trend.
When You MUST Call 911 or Go to the ER
Do not hesitate. Do not try to drive yourself. Call for an ambulance if you have severely high blood pressure AND any of these symptoms:
- Chest pain, pressure, or a squeezing sensation (sign of a heart attack).
- Severe headache, confusion, blurred vision, or difficulty speaking (sign of a stroke or brain swelling).
- Shortness of breath or coughing up blood (sign of fluid in the lungs).
- Severe anxiety, nausea, or vomiting.
- Numbness, weakness, or inability to move one side of your face or body.
- Seizures.
- Severe back pain (could indicate aortic dissection, a tear in your main artery).
When you call 911, say clearly: "I am having a hypertensive emergency. My blood pressure is [state your reading] and I am experiencing [state your worst symptom, e.g., chest pain]." This helps them prioritize and prepare.
What NOT to Do: Dangerous Home "Remedies"
In the age of internet advice, you'll find some terrible suggestions. I've been writing about cardiovascular health for a decade, and I see these myths repeated constantly. Avoid them like the plague during a crisis.
Do NOT take a hot bath or shower. Heat causes your blood vessels to dilate (widen) at the surface, which can cause a sudden drop in blood pressure when you stand up, leading to fainting and injury. It also stresses the heart.
Do NOT "chug" gallons of water or consume massive amounts of potassium (like banana smoothies). While hydration and potassium are good for long-term management, overdoing it instantly can disrupt your electrolyte balance, which is dangerous, especially if organ damage is starting.
Do NOT rely on "instant" supplements like garlic or hibiscus tea. They may have mild, long-term effects, but they are utterly useless and a waste of precious time in a true emergency. They are not potent or fast-acting medications.
The biggest mistake? Focusing solely on the number on the monitor and ignoring the symptoms your body is screaming at you. The number provides context, but your symptoms dictate the urgency.
Beyond the Crisis: Long-Term Management to Prevent Another Emergency
Surviving a scare is a powerful motivator. Here’s how to build a fortress so it doesn’t happen again.
Medication Adherence is Non-Negotiable. Take your prescribed meds exactly as directed. Set phone alarms. Use a pill box. Running out or skipping doses is the most common trigger for a rebound hypertensive crisis.
Invest in a Validated Home Monitor. Look for devices validated by organizations like the American Heart Association or the British Hypertension Society. Get the right cuff size for your arm. Check it against your doctor's device once a year. Track your readings at consistent times (e.g., morning and evening before meds/food).
Build Your Daily Defense:
- DASH Diet: Not just "eat less salt." Emphasize fruits, vegetables, whole grains, lean protein, and low-fat dairy. The DASH eating plan from the National Heart, Lung, and Blood Institute is the gold standard.
- Move Consistently: Aim for 150 minutes of moderate exercise (brisk walking, cycling) per week. It's about regularity, not marathon sessions.
- Master Stress: Find your outlet—daily meditation (try an app like Insight Timer), yoga, or even 10 minutes of quiet reading. Make it a habit, not just a crisis tool.
- Limit Alcohol & Quit Smoking: This is the hardest part for many, but the payoff for blood pressure and overall health is immense.






Leave a comment